Sources – Shafer’s textbook of oral pathology
Image source – researchgate.net , Google images



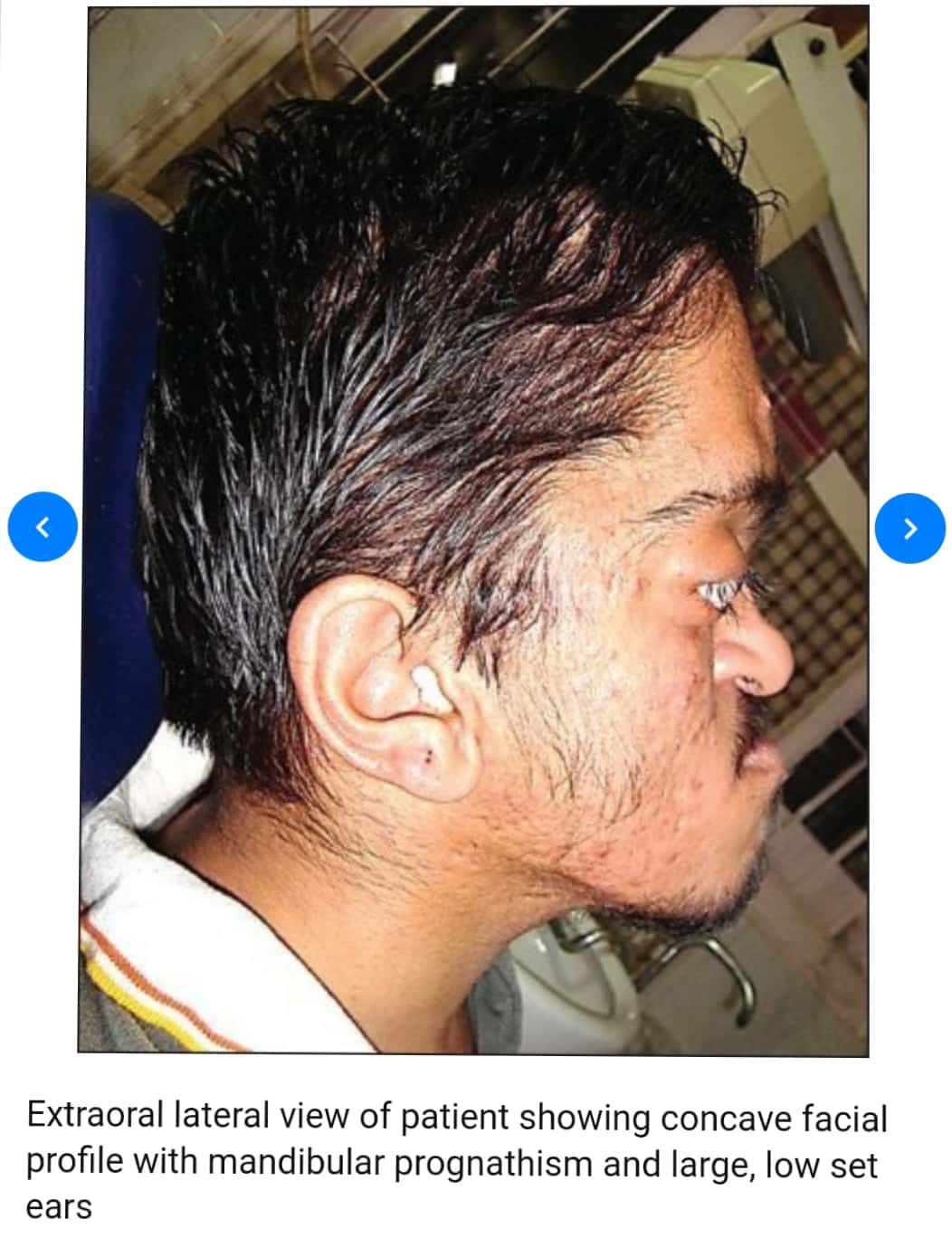
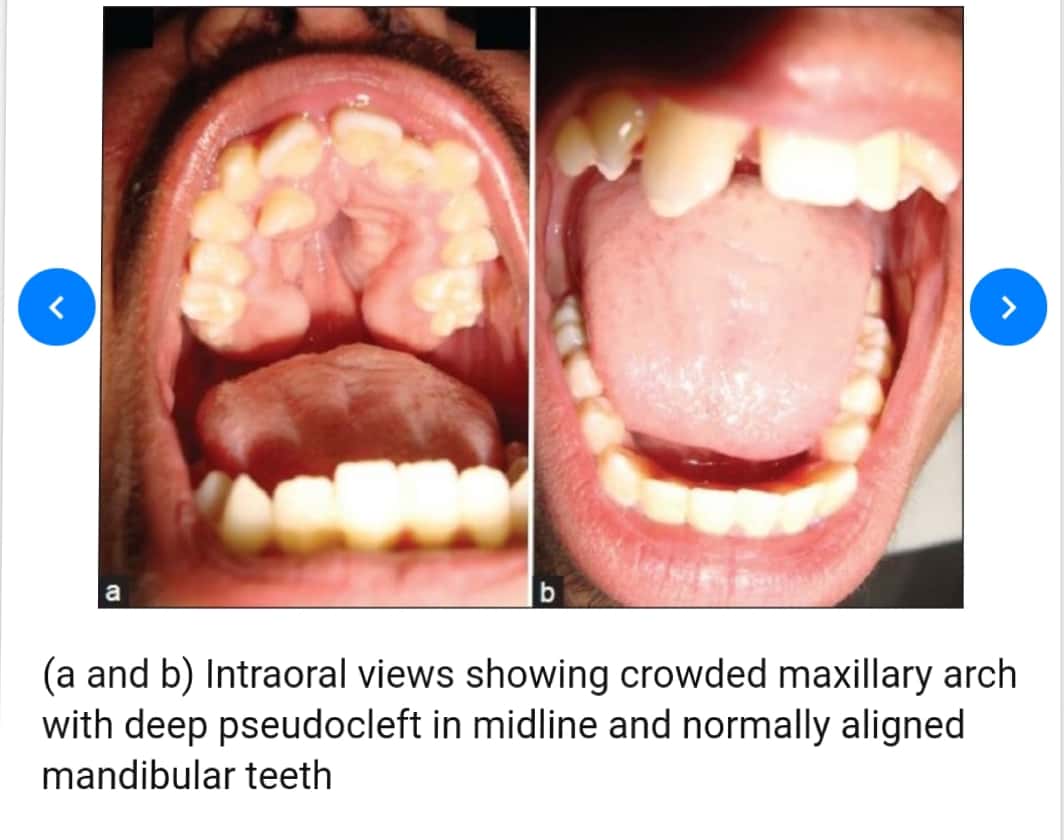




Sources – Shafer’s textbook of oral pathology
Image source – researchgate.net , Google images


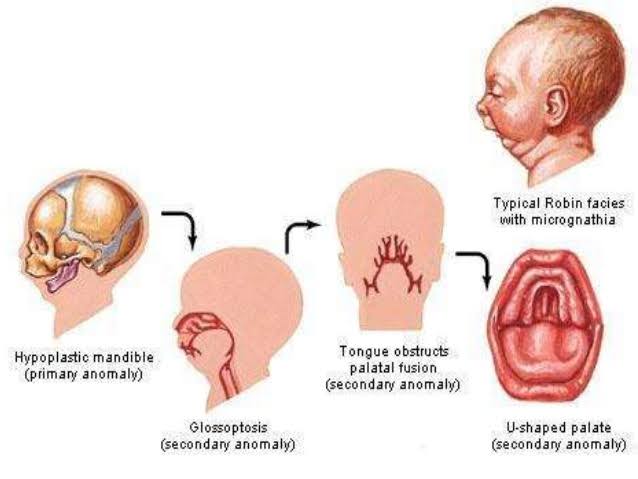

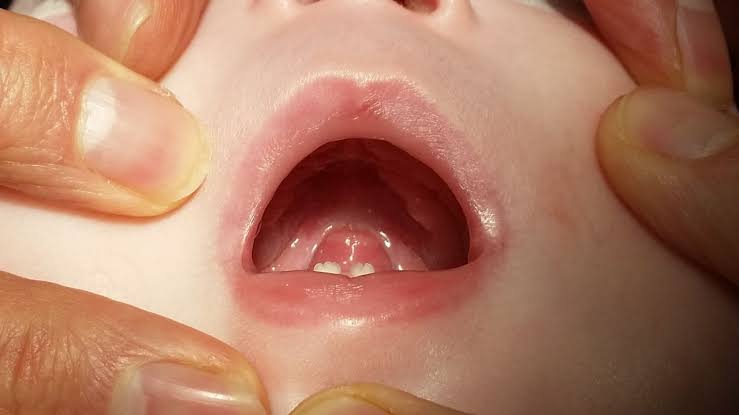




Sources – Shafer’s textbook of oral pathology , slideshare.com
Image source – Google images




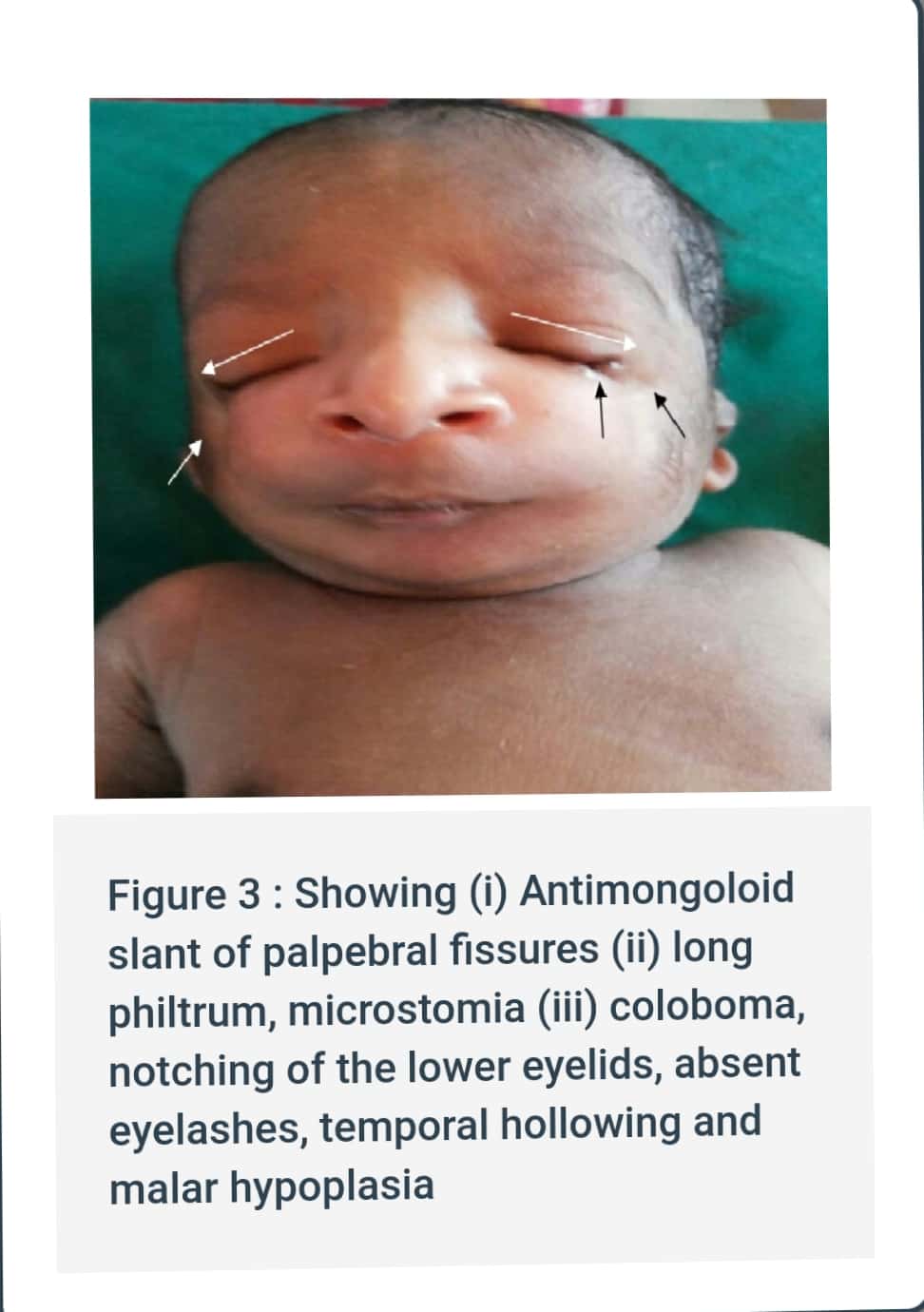

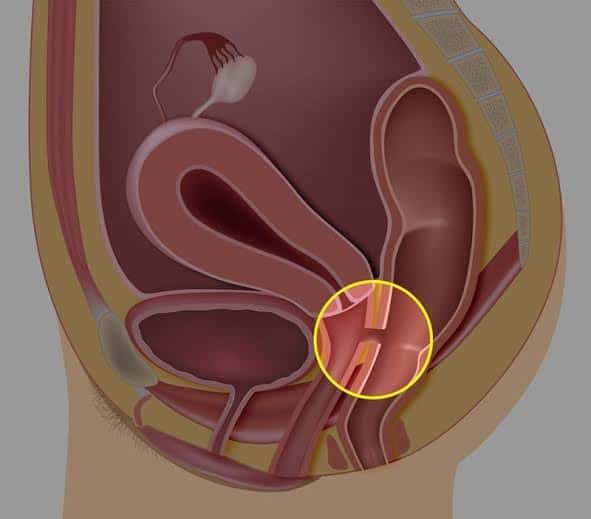
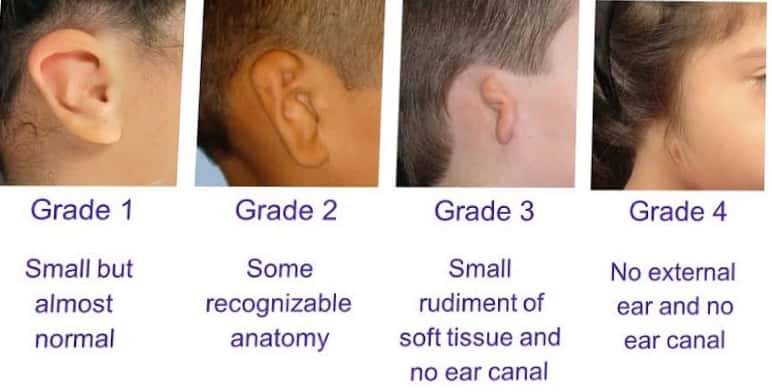





Source : Anil Ghoms textbook of oral medicine , Shafer’s textbook of oral pathology
Image source : Google images
• Also known as PARTSCH II or CYSTECTOMY.
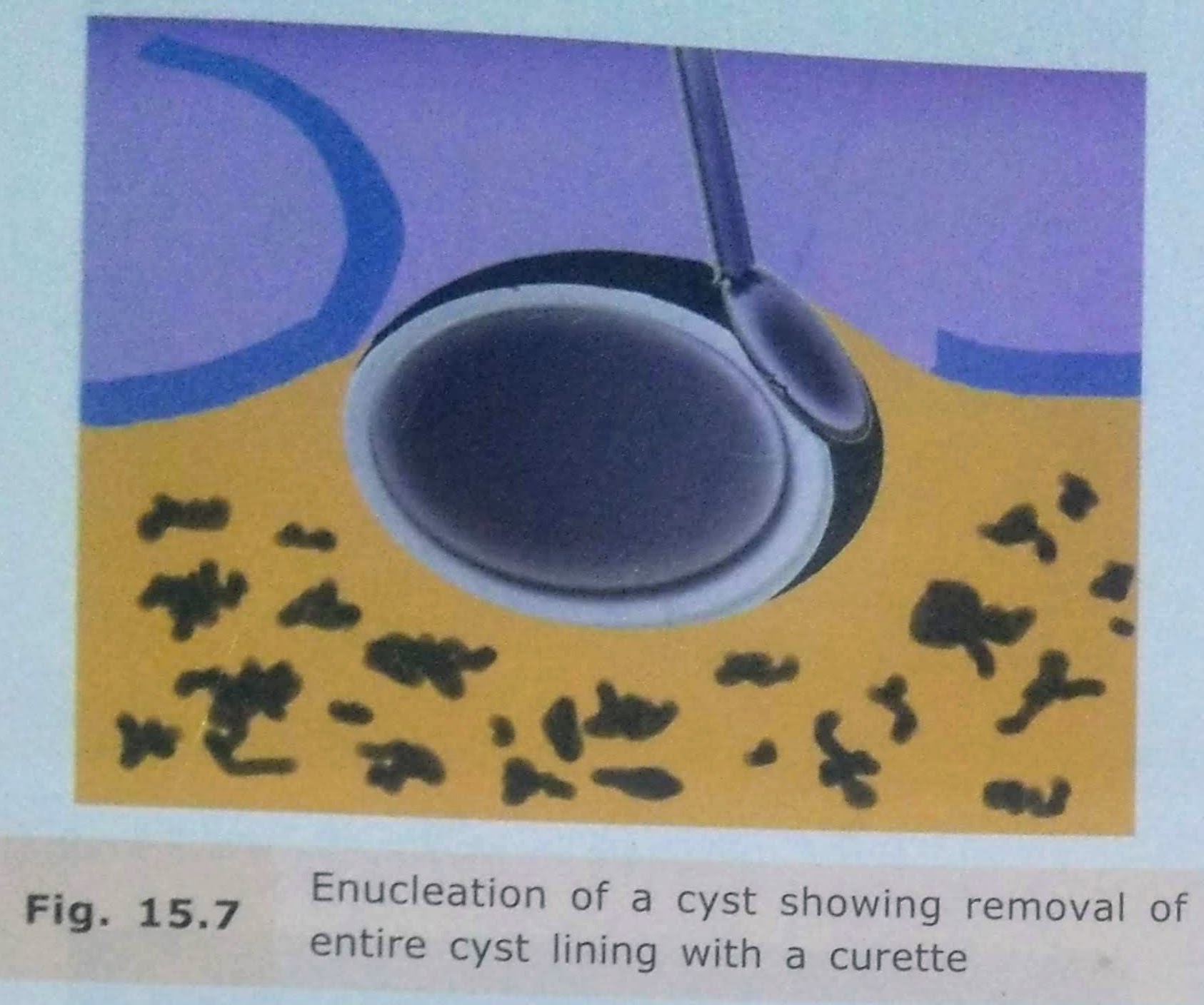
• Enucleation is the surgical removal of the entire cystic lining in to-to.
By definition, it means shelling out of the entire cystic lining without rupture.
This surgical procedure leaves behind a hollow cavity in bone covered by oral mucoperiosteum.
This gets filled up with blood clot which eventually organizes to form healthy bone.
INDICATIONS:
• Is the treatment of choice for removal of cysts of jaws+ should be employed with any cyst of the jaw, that can be safely removed without sacrificing underlying structure.
ADVANTAGES:
DISADVANTAGES:
1.Relatively radical procedure.
2.Chances of devitalising the adjacent teeth.
3.Chances of fracture of the jaw.
4.Risk of creation of oroantral/oronasal communication
TECHNIQUES:
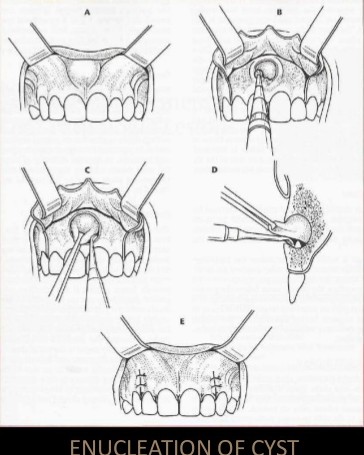
Enucleation with Primary Closure:
• Small cysts can be removed under local anaesthesia
• large cyst should be taken out under general anesthesia, as they are close to vital structures and blood vessels.
• After achieving adequate anesthesia, a mucoperiosteal incision is made such that the incision rests on sound bone.
• Mucoperiosteal flap is reflected taking care not to perforate rate the cystic lining.
• If the bone is perforated by the cyst, the lining will be adherent to the periosteum and will be difficult to reflect it.
• The cystic lining is exposed and now carefully teased away from the bone.
• It is relatively easy to separate the cystic lining from the bone because there is a layer of fibrous tissue between the two which is easily separabl.
• In case of infected cysts or an odontogenic keratocyst. the cystic lining is friable and more difficult to remove entirely.
• Every attempt is made to remove the entire cystic lining in a single piece without perforating it.
• This ensures complete removal.
• After the cyst is removed completely, the cavity in irrigated thoroughly, hemostasis ensured, sharp bone debris are filed and the flap replaced and sutured.
Enucleation with Open Packing :
• In case of a large cyst which was previously infected closure may not be possible
• After enucleation, the wound is then packed with me impregnated with bismuth iodoform paraffin paste (BIPP) or Whitehead’s varnish.
Enucleation with Peripheral Osteotomy:
Enucleation with Bone Curettage:
• After enucleation, if there is a doubt that a part of the line has been left behind, it can be curette out.
• A bone curette is used to scrape the band remove any remaining lining
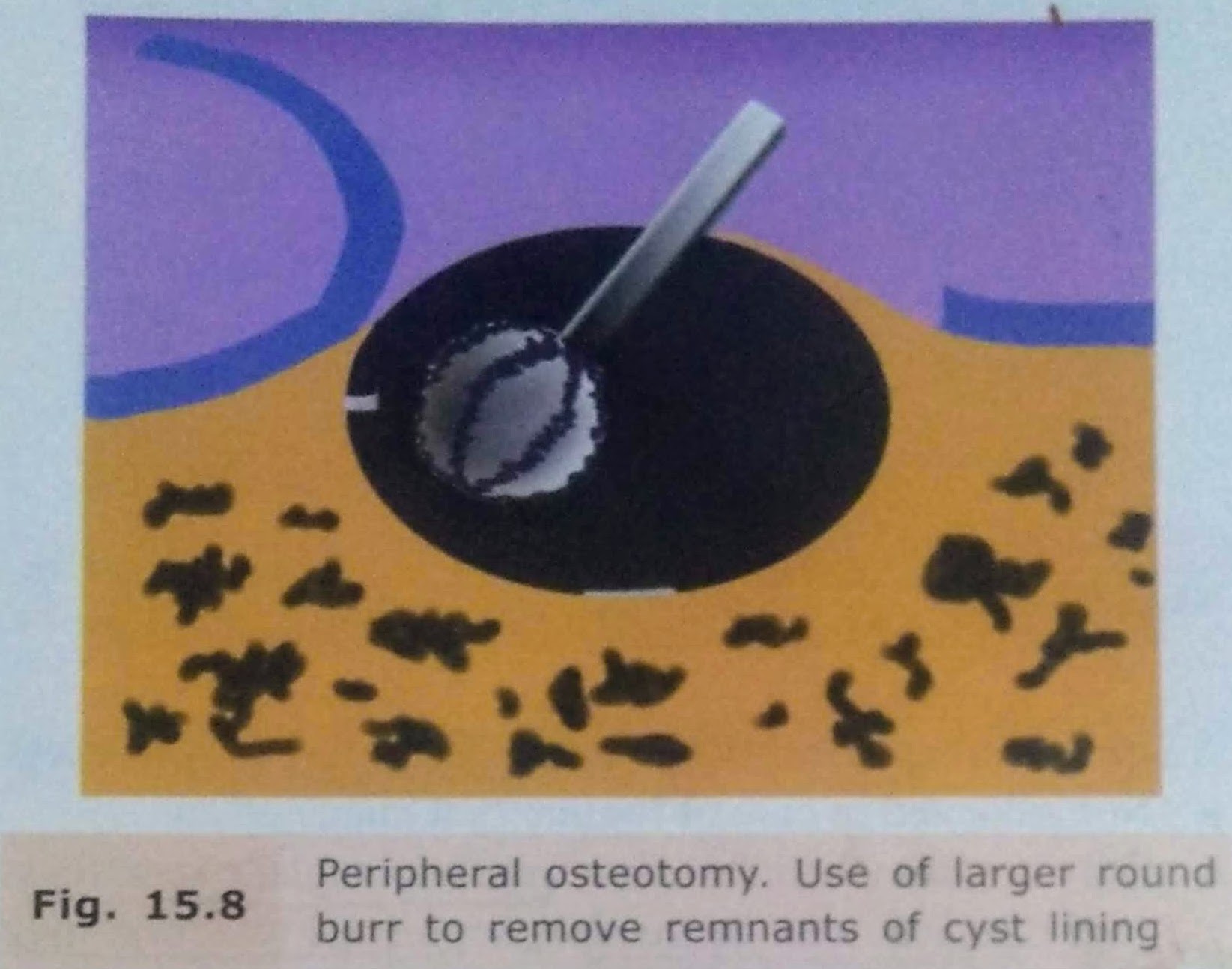
Enucleation with Peripheral Osteotomy
• In this procedure, instead of using a curette, a large round bur may be used to remove around 1-2 mm of bone around the entire periphery of the cystic cavity.
• This is done to ensure that any remaining epithelial cells present in the east wall or body cavity are removed.
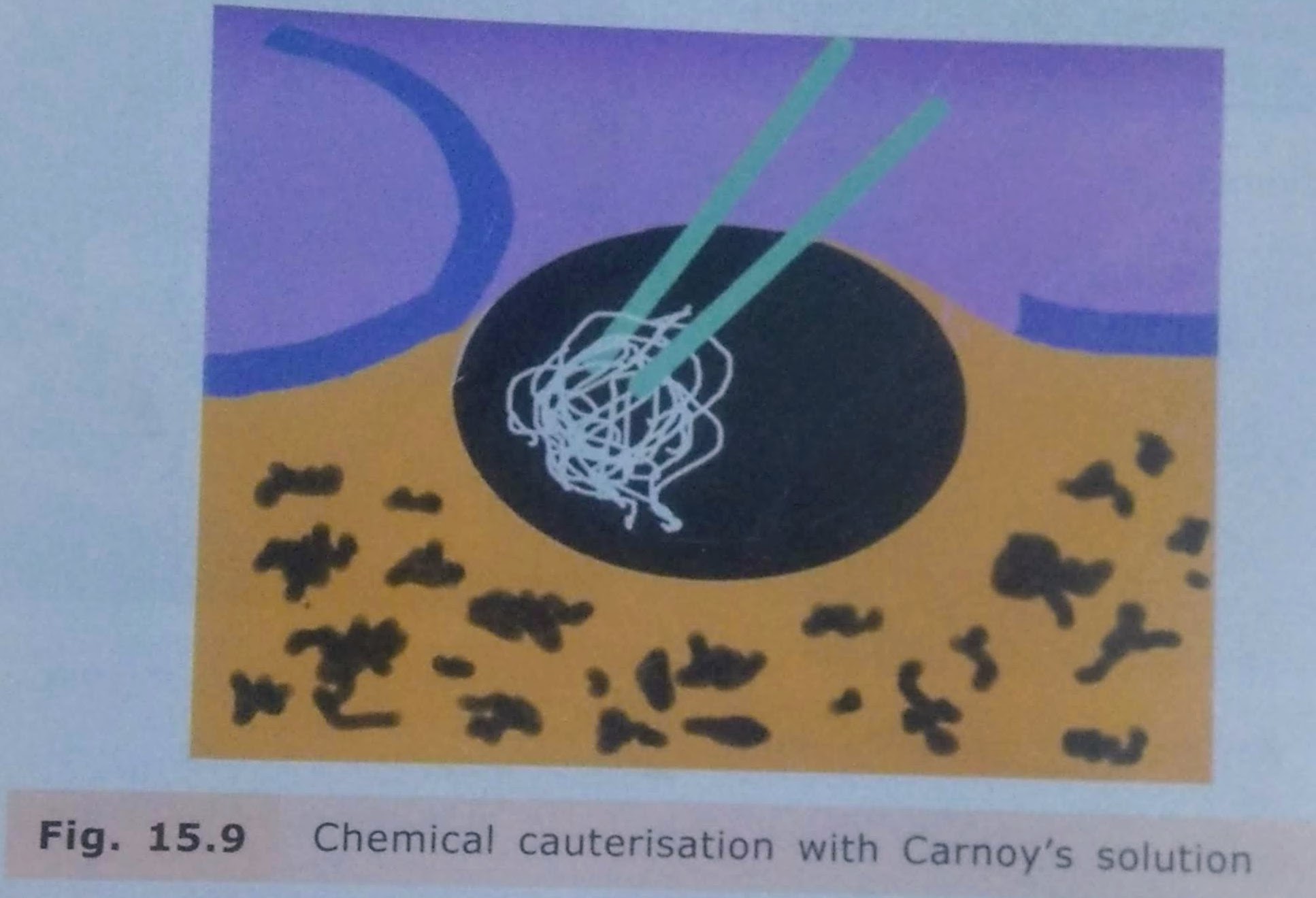
Enucleation with Chemical Cauterisation:
• It is indicated mainly in cases of odontogenic keratocyst.
• After enucleation, to remove any remaining lining of the cyst chemical cauterising agent Carnoy’s solution is applied along the walls of the cystic cavity.
• It is left for about 5-7 minutes and then irrigated thoroughly with saline.
• This solution chemically cauterizes any remaining cells of the system.
Enucleation with Bone Grafting
• Bone grafting with autogenous cancellous bone grafts can be done in case of large bony defects.
• The bone graft obliterates the cavity and stimulates osteogenesis.
• There is, however, a risk of wound breakdown and infection of the bone graft which may lead to failure.

COMPLICATIONS:
• Risk of bone fracture due to cyst.
• Inferior dental nerve involvement.
• Management of teeth related to cyst.
• Oroantral Communication.
• Hematoma formation.
• Infection.
• Dead Space: At surgical procedure, a hollow dead space is formed. It is usually filled up with blood clot and eventual bone formation.
However, there are chances of infection of the clot, breakdown of suture line and pus discharge.
REFERENCES:
• Textbook of Oral & Maxillofacial Surgery, Chitra Chakravarthy (2nd Edition)
• SlideShare



















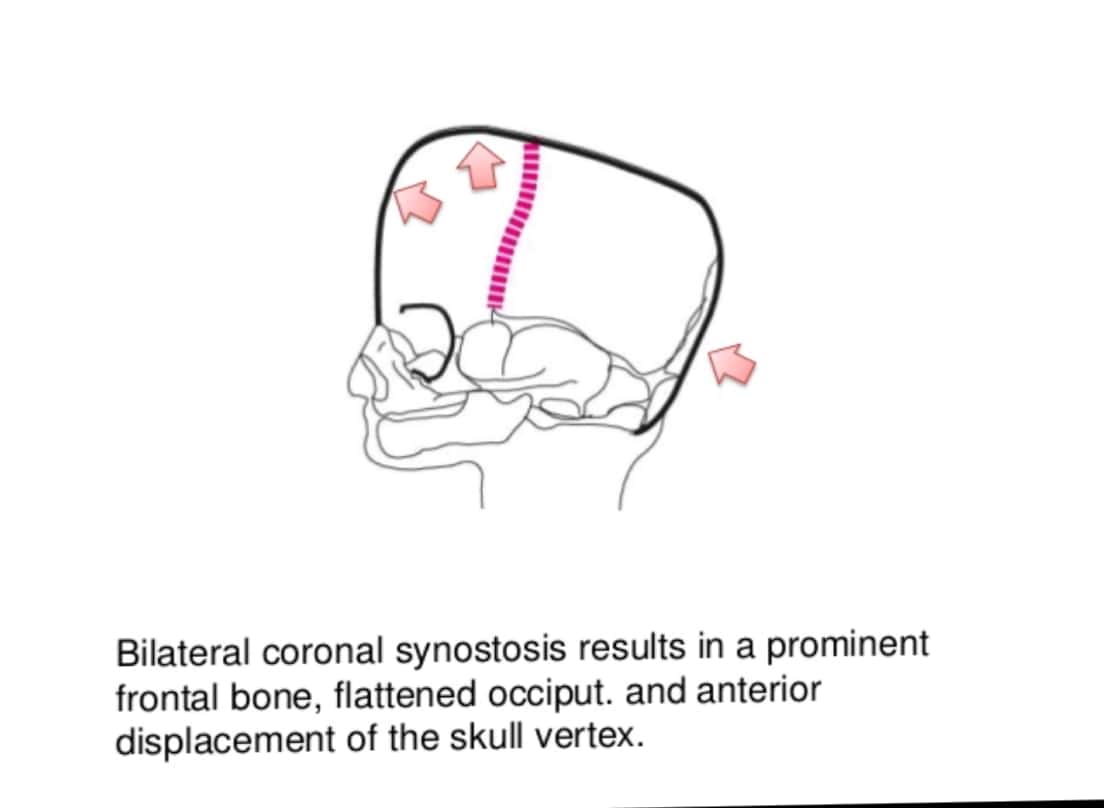








Sources – Shafer’s textbook of oral pathology , slideshare.com
Image source – Google images , researchgate.net

MARSUPIALIZATION:
• PARTSCH(1892) described a type of compression procedure for treatment of cyst.
• Also k/a PARTSCH I OPERATION & CYSTOTOMY.
• In this procedure a window/fenestrations made in the bone and cystic content is evacuated.
• The cyst lining is left behind.
• Once the cyst contents are evacuated, the intracystic pressure reduces.
• Hollow cavity is packed till it gets obliterated by bone over a period of time.
• The cystic lining then becomes continuous with normal oral mucosa.
INIDICATIONS:
• In extremely large cysts.
• Risk of cyst opening into maxillary sinus/nose due to surgical removal of complete lesion.
• In very young patients, where it will permit eruption of enclosed tooth,underlying developing tooth.
• Patient with poor general condition for allowing minimal surgical procedure.
• In cases, where surgical procedures may cause pathological fracture of jaws.
TECHINQUE:
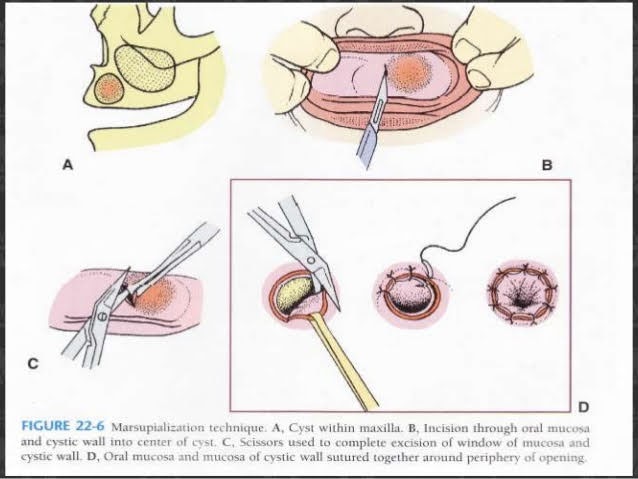
1) Anaesthesia
2) Aspiration
3) Incision: Circular, oval or elliptical. Inverted U Shaped incision with broad base the buccal sulcus. Mucoperiosteum is reflected in this case.
4) Removal of bone
5) Removal of cystic lining specimen
6) Visual examination of residual cystic lining
7) Irrigation
8) Suturing of cystic cavity.
• Cystic lining sutured with the edge of oral mucosa.
• In Y Shaped incision the mucoperiosteal flap can be turned into cystic cavity covering the margin.
• The remaining is sutured to oral mucosa.
9) Packing- Prevents food contamination & covers wound margins. Done with ribbon gauze soaked with WHITEHEAD VARNISH
COMPOSITION
• Benzoin – 10g
• iodoform-10g
• Storax -7.5g Balsam of Tolu -5g
• Solvent ether to 100ml
Pack removed after 2 weeks.
10) Maintenance of cystic cavity
Instruct the patient to clean and irrigate the cavity regularly with oral antiseptic rinse with a disposable syringe.
11) Use of plug:
• Prevents contamination, Preserves patency of cyst orifice.
• Plug should be stable, retentive and safe design.
• Should be made of resilient material (to avoid irritation) like acrylic.
12) Healing:
• Cavity may or may not obliterate totally. Depression remains in the process.

ADVANTAGES:
• Once the cystic lining is evacuated, there is a tendency of the cystic lining to contract. This stimulates endosteal bone formation.
• Marginal ingrowth of normal mucoperiosteum occurs as the cystic lining shrinks. It provides with additional bone regeneration factors.
• Not much surgical skill is required.
• No risk of oroantral/oronasal fistula.
• No damage to adjacent vital structures.
• No risk to adjacent vital tooth.
DISADVANTAGES:
• Entire pathological tissue is left behind.
• High chances of recurrence.
• As the bony cavity is large, healing and filling up with normal bone takes longer time.
• Use of cyst plug is required with repeated cleansing.
• Time consuming & repeated appointment for patients.
REFERENCES:





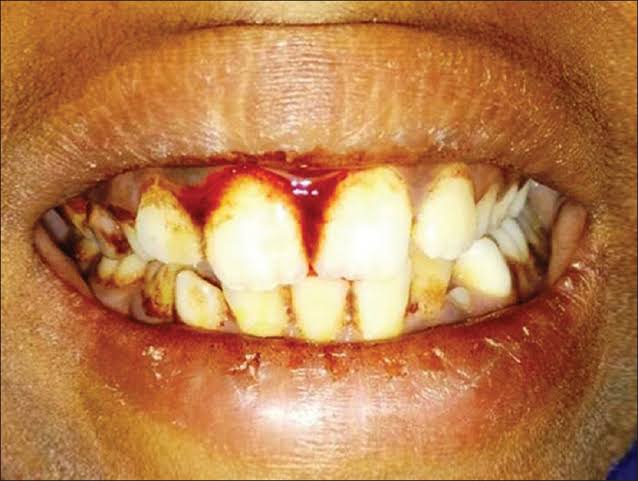


Sources – Shafer’s textbook of oral pathology
Image source – Google images



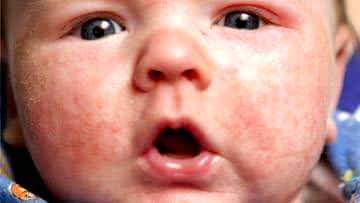


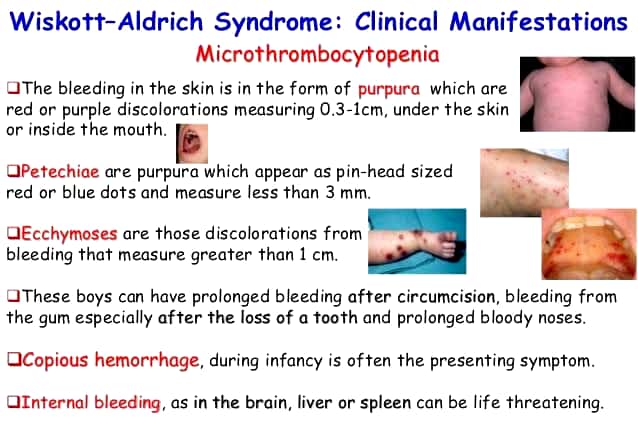


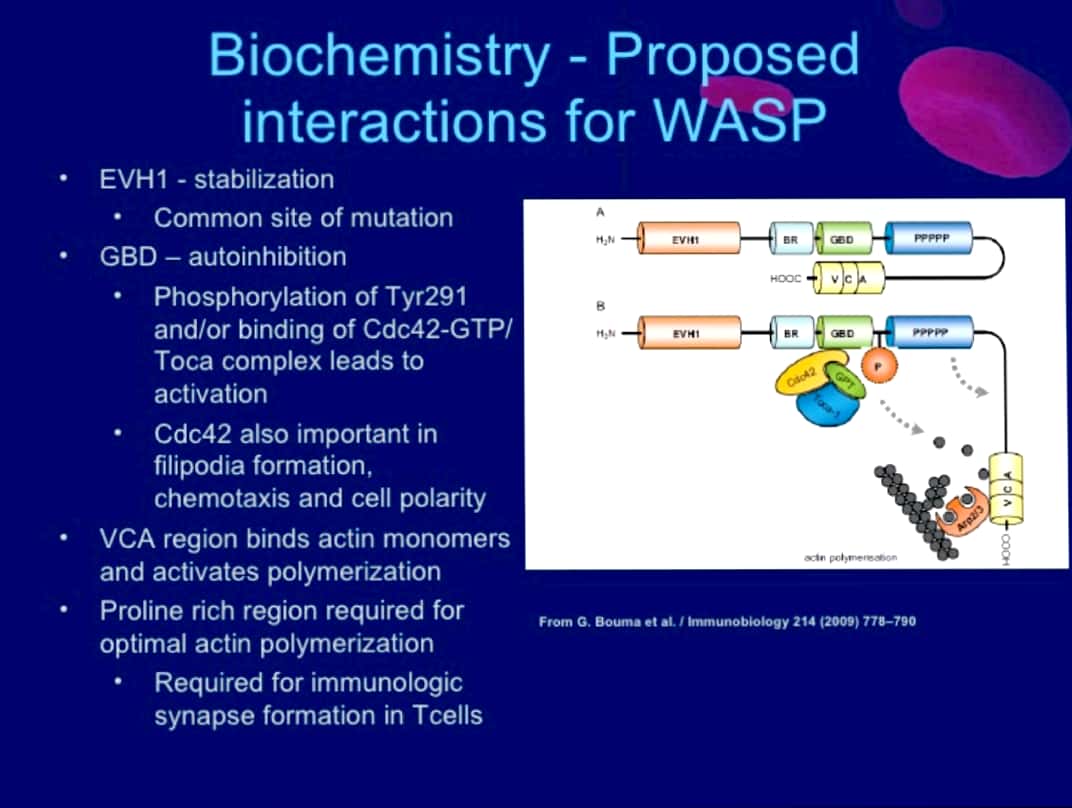


Sources – Shafer’s textbook of oral pathology , osmosis.org
Image source – Google images
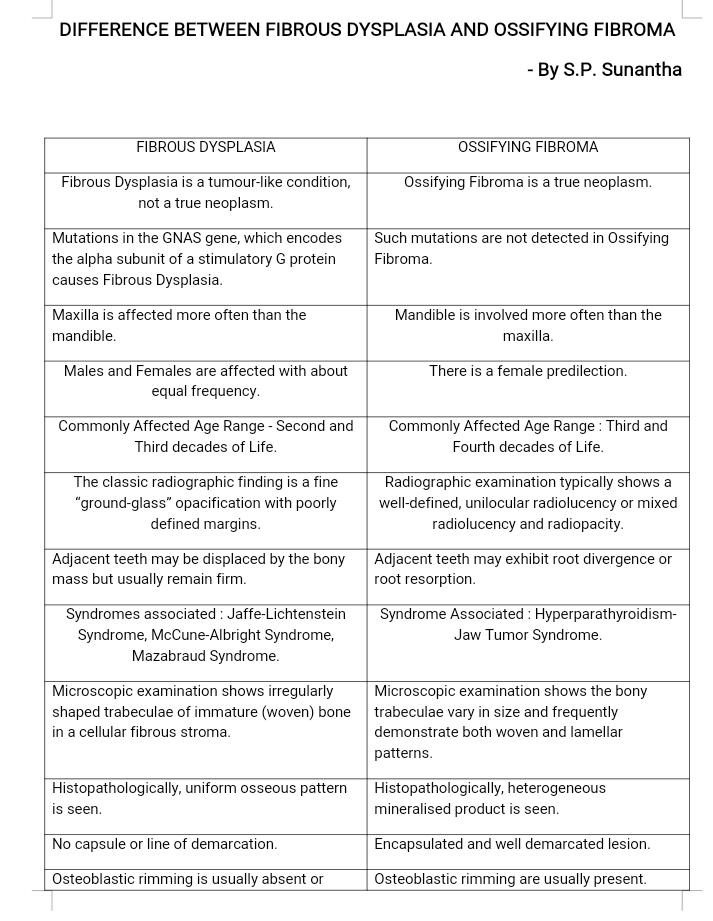

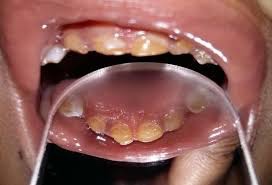
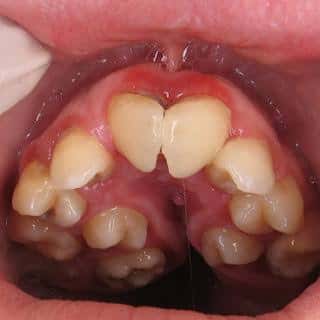
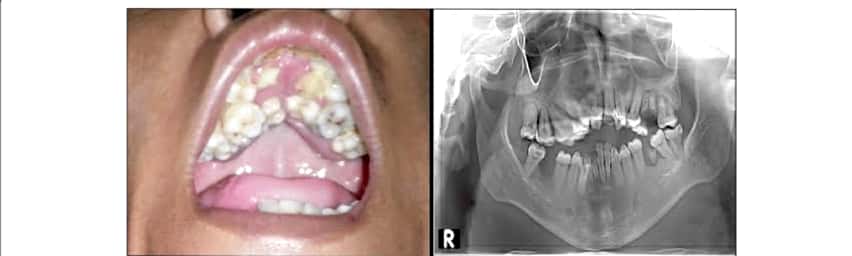
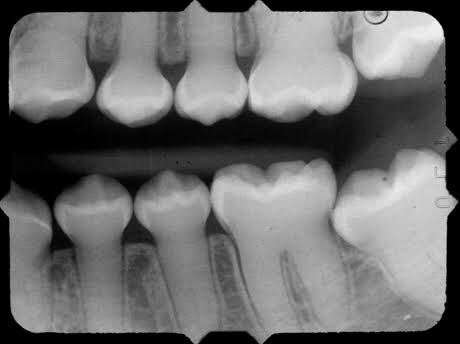
👉🏻 The affected teeth (both dentitions) are grey to yellow brown with broad crowns and constriction at cervical area resulting in tulip shape.
👉🏻 The enamel is easily broken, exposure of dentin ➡️ accelerated attrition.
👉🏻 Normal non-mineralized pulp chambers and canals
👉🏻 This condition is inherited in an autosomal dominant pattern, as a result of mutations on chromosome 4q21, in the dentine sialophosphoprotein gene (DSPP).

👉🏻 Mesodermal disturbance.
👉🏻 Dentin composed of irregular tubules with large areas of unclassified matrix. The tubules are larger in diameter & less numerous.
👉🏻 Odontoblasts – dentinal matrix not layed properly & they are entrapped within this matrix.
CHEMICAL FEATURES:
• Increased water content (60 times the normal)
• Decreased inorganic content
Dr. Mehnaz Memon🖊
References: