

mnemonics





gingiva
gingiva is anatomical term for gums. found in the oral cavity of human being surrounding part of teeth
















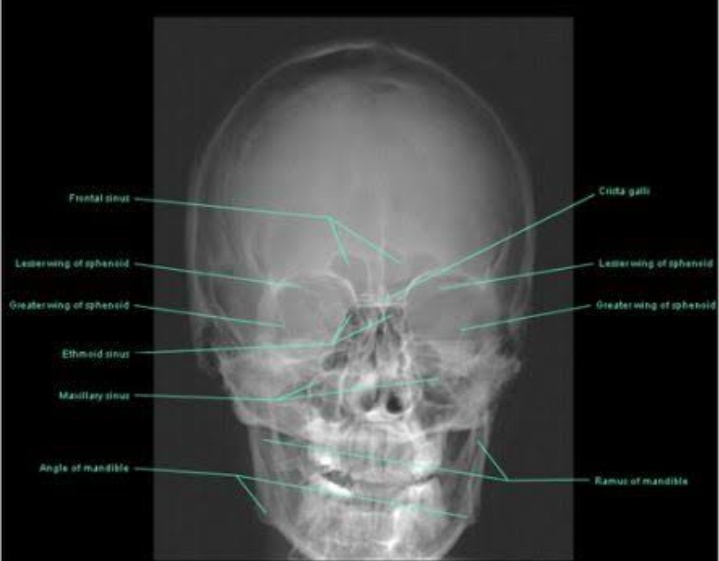
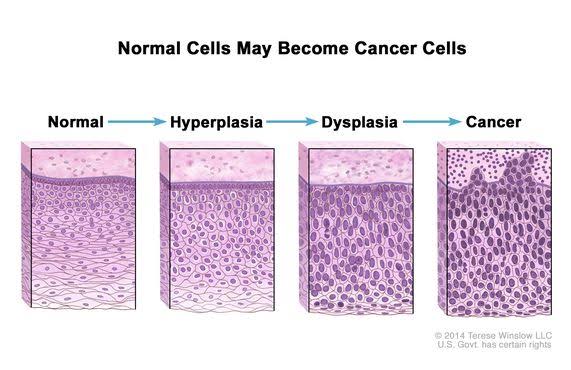
Dysplasia defn- Characterized by loss of uniformity of individual cells and loss of their architectural orientation.
At cellular level- known as atypia
At tissue level-dsyplasia


References- Shafers book of oral pathology 9th edition
Essentials of Oral pathology-Purkait 3rd edition
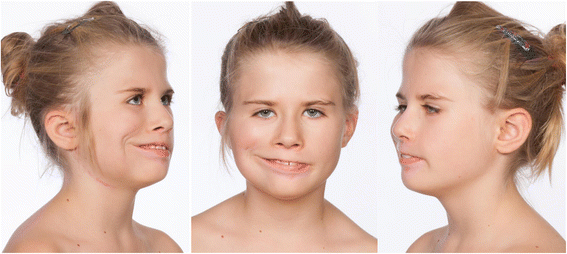



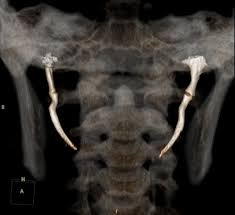



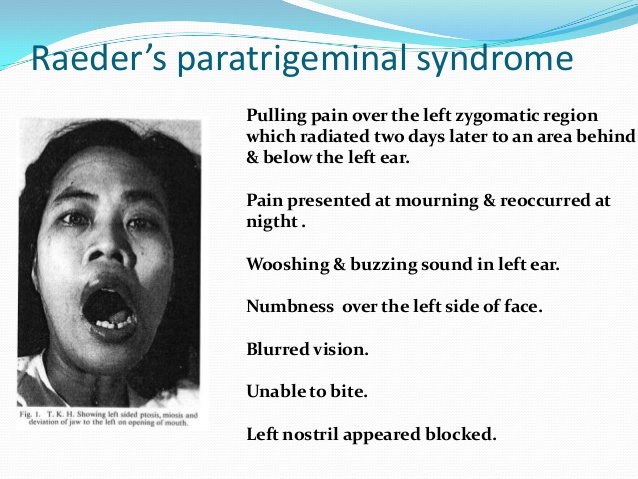
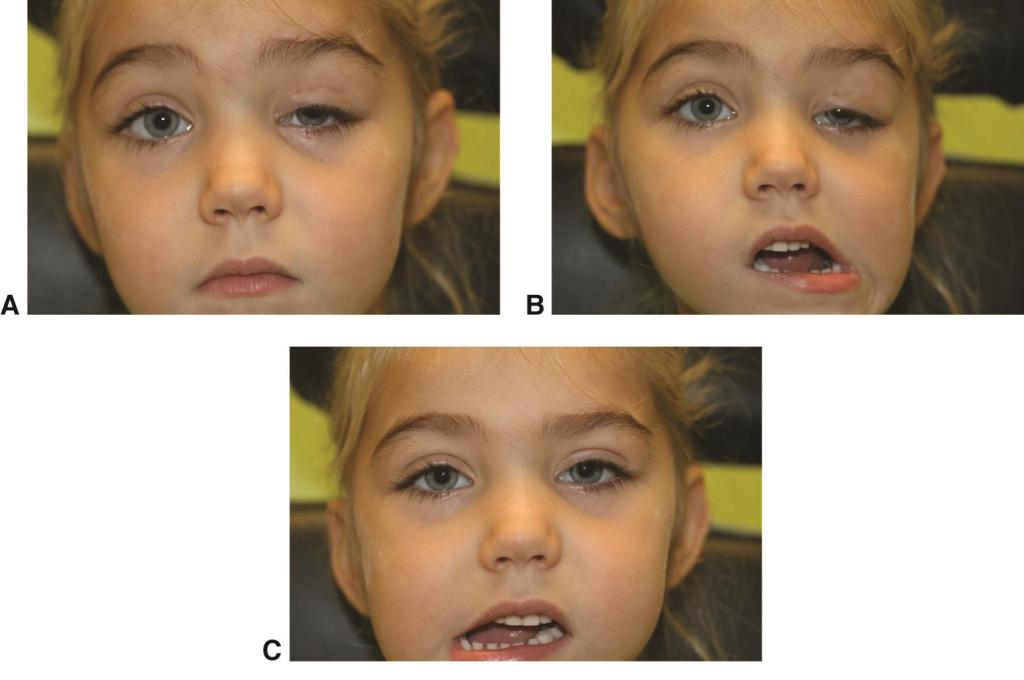
Definition of syndromes are extracted from Dental pulse 13th edition.

Reference Pulse edition 14
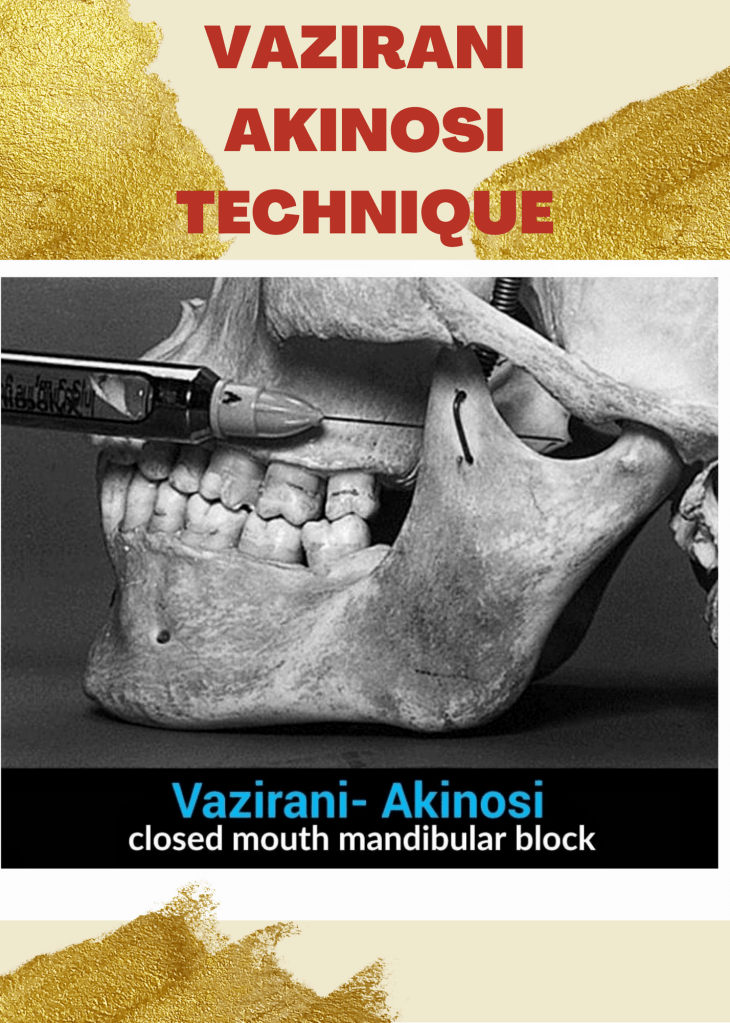
❇️ The Vazirani-Akinosi technique:
🔆“It is a specific method of nerve block in the mandibular region, carried out with the mouth closed.
❇️ The area of distribution of the anaesthesia includes
a) the corresponding dental arch,
b) the body of the jaw and the inferior ramus,
c) the gingiva/mucosa and vestibular periosteum, anterior to the mental foramen
d) the area of distribution of the lingual nerve: 2/3 of the anterior of the tongue and floor of the mouth, the gingiva/ mucosa and lingual periosteum.
🔆» The main indication, already anticipated, is trismus: classically this is contraction of the masticatory musculature which prevents the performance of effective inferior alveolar anaesthesia, for example, in cases of pulpitis or an abscess of a lower molar.
– By Dr. Sneha poeghal , Mallareddy institute of dental sciences , hyd .
References – Malamed


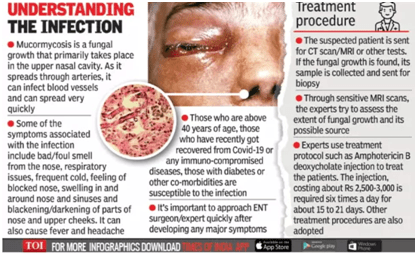
TRANSMISSION
Transmission occurs through three modes: inhalation, inoculation, or ingestion of spores
Mucormycosis infection in the clinical environment has been linked to use of adhesive bandages, wooden tongue depressors, hospital linens, negative pressure rooms, water leaks, poor air filtration, non-sterile medical devices, and building construction. This is a possible explanation for the recent rise in the number of mucormycosis cases during the covid outbreak.
RISK FACTORS FOR MUCORMYCOSIS
Common predisposing factors include-
Depending on the location of fungal infection, mucormycosis is of 5 types-
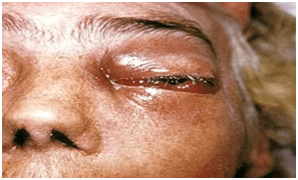

Rhinocerebral form is the most common, accounting to nearly one-third of all the recorded cases of zygomycosis. This type of infection is primarily present in people with uncontrolled diabetes and those who had a kidney transplant.
Symptoms of Rhinocerebral Mucormycosis include-
Symptoms of pulmonary mucormycosis include-
WHAT SHOULD THE DENTIST LOOK OUT FOR?
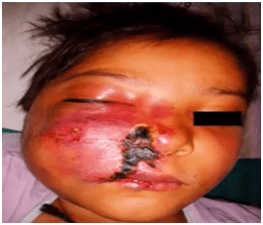

The commonly involved areas are the palate, face, eyes and the nasal passage. Some of the signs include-
DIAGNOSIS

Early diagnosis of mucormycosis infection is very crucial because of its rapid progression. Tools that help in making proper diagnosis are-
Radiographically, rhinocerebral mucormycosis shows nodular thickening of the sinus necrosis, sinus opacification without fluid level and spotty destruction of paranasal sinuses. CT scan with contrast/magnetic resonance imaging (MRI) can demonstrate erosion or destruction of bone and may help to determine the boundary of the disease.
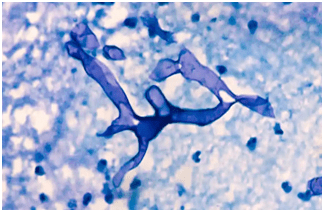
Histological examination of the biopsy specimen using KOH staining is useful in giving the final confirmation of the presence of fungal infection,which demonstrates long, broad, branching and nonseptate fungal hyphae. It is detected via a cotton swab sample of the nasal cavity, which is examined under a microscope.
COVID ASSOCIATED MUCORMYCOSIS
The mucormycosis cases reported after covid infection in a patient due to covid treatment related immunosuppression is called Covid-Associated Mucormycosis (CAM). Black Fungus is now commonly seen in patients who have recovered from covid-19 infection, who have been on oxygen support for a long time and diabetic patients. An infected mouth mask or an oxgen mask could also be the cause of the disease.
The fungus is normally present in the mucous lining of a healthy person, but a drop in the immune defense can trigger the growth of the fungus. After that it can reach to vital organs such as sinus, lungs and even brain. This is now happening more due to the heavy dose of steroids and anti-viral drugs which are used in the treatment of covid patients.
Diabetes further complicates the situation and promotes rapid fungal growth. The spread of the fungal infection is very aggressive and contagious in diabetic patients because of disruption of host defense mechanism and increased availability of nutrients such as free iron.
While steroids help in reducing lung inflammation to overcome the harmful effects of coronavirus, they also reduce immunity and cause a hike in blood sugar levels in both diabetics and non-diabetic Covid-19 patients. Thus, it is believed that this decline in immunity could be the driving force behind the rapidly increasing cases of mucormycosis.
TREATMENT OF MUCORMYCOSIS
The three main anti-fungal medicines employed in the treatment of Mucormycosis are-
In majority of the cases, surgical removal of the infected tissue is the only treatment option. Since there are high chances of reemergence of the fungal infection, it should be monitored carefully, with frequent follow-ups. Broadly speaking, the target organs of this fungal infection are eyes, lungs, skin and most recently, the oral cavity. This fungal infection is highly contagious as it spreads rapidly to other organs of the body, particularly to the brain.
Some simple oral hygiene practices to avoid the chances of getting mucormycosis after Covid infection are-

Maintaining good oral hygiene
Recent studies have proved that the anti-viral medicines and the steroids taken during the Covid infection period, lead to rapid growth of bacteria and fungus in the oral cavity, post recovery. This can cause a serious threat to the sinus, lungs, and even the brain. Routine brushing at least twice or thrice a day may help you to control the bacteria. Oral rising using a suitable mouthwash can also prove to be very beneficial.
New Toothbrush
It is advisable to the patients to change their toothbrush after recovery to avoid chances of reinfection from the virus present on the old toothbrush.
Disinfecting the toothbrush and tongue cleaner
Some experts suggest that a patient who has recovered from covid infection, should not keep their toothbrush and tongue cleaner in the same holder as of their other family members. This can help in spread of infection to other members of the family. It is also advised to clean the brush and tongue cleaner using an antiseptic mouthwash.
ROLE OF A DENTIST
Dentists can play a very important role in management of mucormycosis by diagnosing it early, carrying out proper investigations and referring to the appropriate specialists at the correct time. They can keep in mind the following clinical workflow for mucormycosis, to detect such cases coming in their clinics at their earliest-
History– A dentist should properly take history of previous Covid infection and hospitalization.
Symptoms and signs– A dentist should look out for the signs which have been mentioned previously
Investigations– Performing adequate investigations such as CT, MRI, Biopsy, etc.
Prescribe– A dentist can prescribe Analgesics and anti-inflammatory drugs, Antipyretics and Antibiotics to provide the patient relief for a shorter period, before referring to specialists.
Counselling– Counsel the patient to stay calm and follow the instructions.
Record– A dentist should keep a record of the clinical findings and the referrals.
Referral– A dentist should refer the mucormycosis patients to OMFS, ENT and Ophthalmologist for appropriate treatment.
Mucormycosis does not spread via contact transmission. Thus, the best way to keep oneself safe from the fungal infection is by self-care. One should always wear a mask before stepping outdoors even if their immunity is good. For health care professionals, it is very important to wear masks and gloves while doing bandages on the wounds and even while tending to fungal infected patients, to keep themselves safe.
DR. DEVYANI ALLEN
BDS, FRCD
Invisalign or clear aligners are orthodontic devices that are transparent, plastic form of dental braces used to adjust teeth.

They are designed as follows :
Each aligner is intended to be worn an optimal 2 hrs a day for one to two weeks. On average, the treatment process takes 13.5 months although it varies based on complexity of planned teeth movements.
Cost of clear aligners in India ranges from 1,50,000-3,50,000.
Pros of invisalign :
Cons of invisalign :
Quaffing and boozing have become common in almost all over the world. It does has a deleterious effect on liver but does it effect teeth too? Oh yes!!! it does has a role in effecting oral cavity in wide ways. Let us quickly go through it’s action.


How can we avoid such deleterious effects?? Well!! here are few tips :

References : wcdentalarts.com, deltadentalins.com, covingtondentalcenter.com