SOURCE – RAMYA RAGHU TEXTBOOK


SOURCE – RAMYA RAGHU TEXTBOOK
As private practice is one of the huge forms of practice in India for dentists, bleeding is an important complication encountered day in and day out. The idea of this post is to just have a Gist in the post Extraction bleeding control,many techniques are followed by many clinicians.so no technique is the gold standard for the control of Extraction bleeding.
In a clinical perspective, basics of bleeding control is proper evaluation of the preoperative blood investigation. It should be made mandatory for any kind of procedure either be a impression making or invasive oral surgery. Basic blood picture should comprise of CBC,BT,CT,PT, Thromboplastin Time, Complete Blood Sugar (CBG). Many ignore advising of PT and Thromboplastin Time but it can reveal bleeding disorders like hemophilia. If you suspect the patient to be having any renal or hepatic impairment do not hesitate to order for LFT and RFT. Though these tests cost some amount it’s important that patient is not harmed by our negligence after our procedure.
Post extraction bleeding is one of the commonest emergency for every dentist in a clinical setup. It can be arrested with packing of gel sponge and closing the area with sutures,if the Extraction site had not been closed with sutures.close inspection of the socket should be done and the previous formed clot in the socket should be retracted or removed by irrigation of the socket first with saline then with betadine and finally with again saline. After the induction of fresh bleeding from the socket pack the area with gel sponge and suture the socket. This gel sponge can degrade by itself ,so there will not be any need for reexploration of the site. There are many day to day update in the management of bleeding and new hemostats and hemostatic techniques are developing.
In cases where the haemostasis is not achieved even after the closure of the socket suspect for a systemic cause which might have been missed during pre-op evaluation.patients on oral anticoagulants usually have irreversible action of prevention of aggregation of Thromboxin A2 which is responsible for platelet aggregation.Even aspirin and Acetaminophen have revesible inhibition of Thromboxane A2. This history to be noted. Bleeding disorders like hemophilia A ,B,C can invlove the deficiency of the clotting factors hence, the PT and thromboplastin time can be prolonged. Vitamin K Antagonist therapy patients, malnutrition patients are suseptible to uncontrolled bleeding.
Proper evaluation of the patient preoperatively and keeping the conditions which can cause bleeding are to be kept in mind so that the clinician can rule out a diagnosis and refer to the appropriate specialist.
Common causes of bleeding which should always be in mind
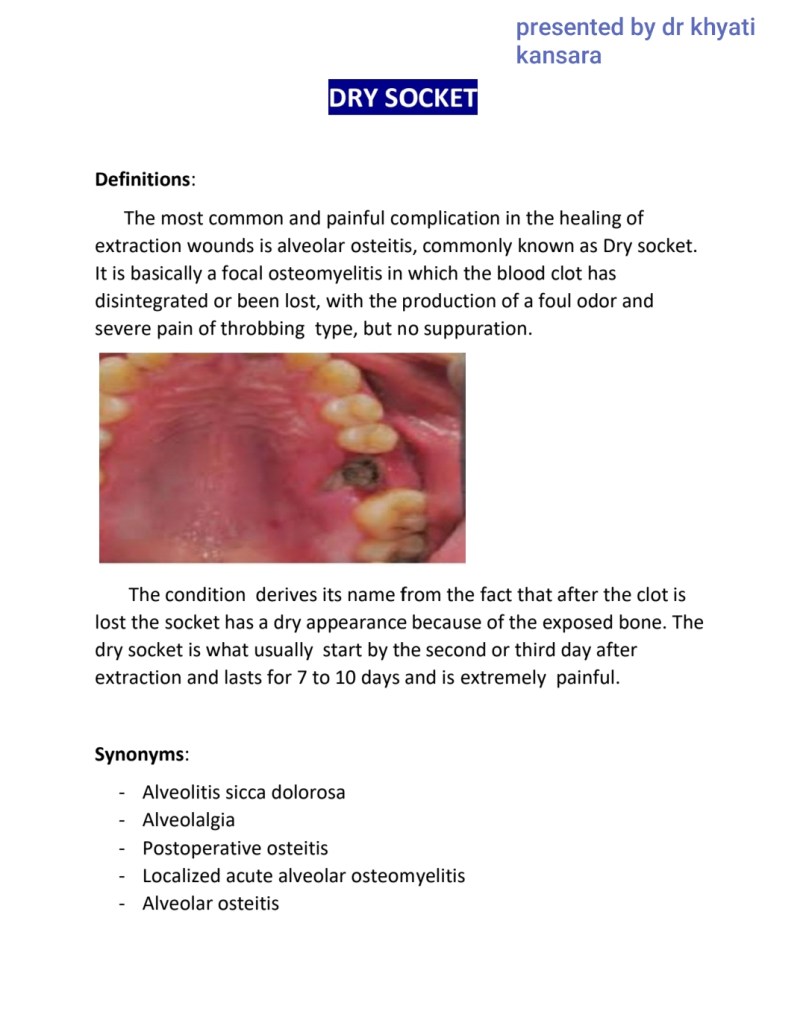




SOURCE – RAMYA RAGHU TEXTBOOK

SOURCE – RAMYA RAGHU TEXTBOOK

SOURCE – RAMYA RAGHU TEXTBOOK


SOURCE – RAMYA RAGHU TEXTBOOK

SOURCE – RAMYA RAGHU TEXTBOOK
Female:
Male: