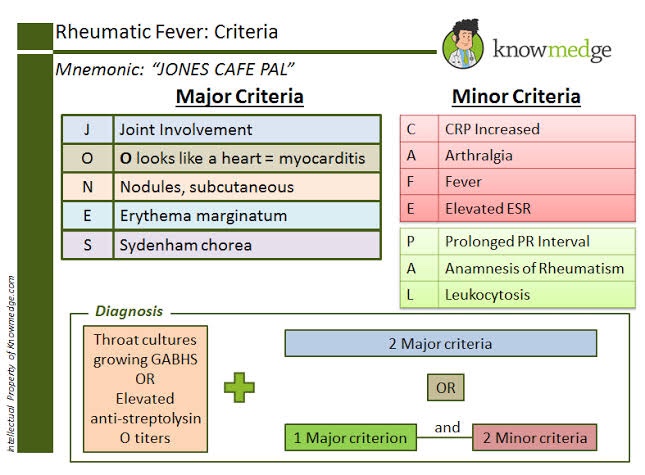
References:
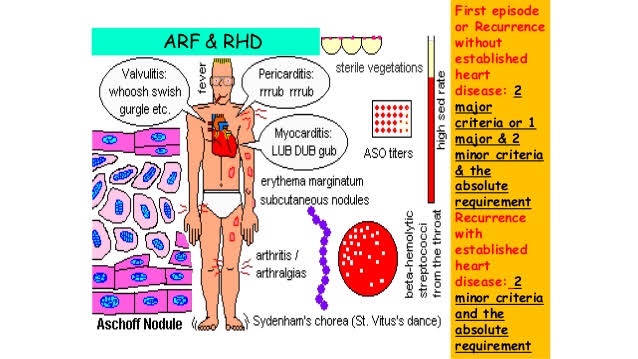







References:
Tap to View in full size…⬇️





References: Phillips Science of Dental materials 12th Ed.

Leukemias are malignant Neoplasms of the haematopoetic stem cells characterized by diffused replacement of bone marrow by Neoplastic cells with or without involvement of the peripheral blood.
➡️ Chronic leukaemia is a disease of insidious onset, affecting middle aged & young adults (CML)
🔘 1 lakh - 5 lakh/cu.mm
🔘 Differential count reveals more mature forms in Peripheral smear, complete spectrum of granulocytes, myelocytes & band cells (50%)
🔘 Blast cell > 10% of leukocytes
🔘 Phases:
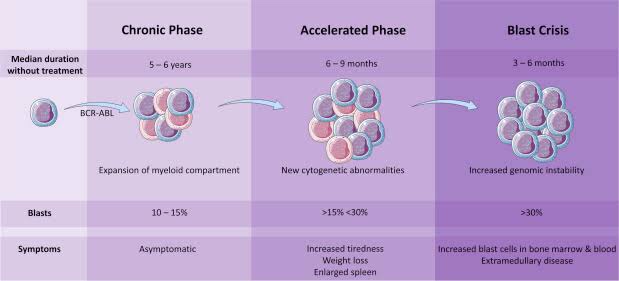
1. Chronic phase:
➡️ Myeloproliferative disorder – excessive proliferation of myeloid cells & mature segmented Neutrophils
➡️ Basophils upto 10% (feature of CML)
2. Accelerated phase:
3. Blastic phase: Myeloid blast crisis in CML resembles AML >20%
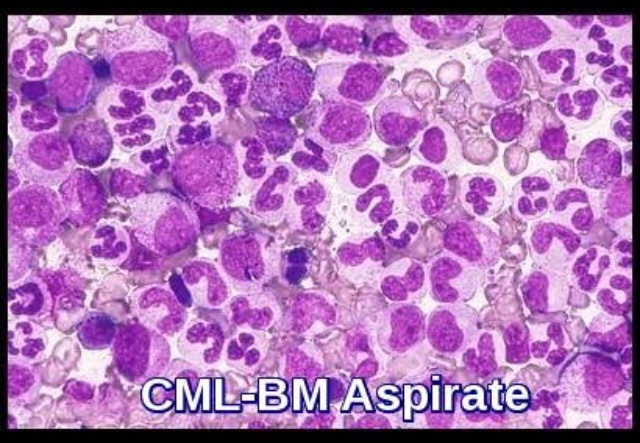
• neutrophil alkaline phosphatase (NAP) activity is markedly reduced in CML
🔘 Splenectomy and splenic irradiation have been used in patients with large and painful spleens, usually in the late phase of CML. This is rarely needed in patients whose disease is well controlled.
🔘 For those patients unable to tolerate chemotherapy, leukapheresis is a viable option.
Dr. Mehnaz Memon🖊
References:

There are four stages in the repair of a broken bone:👇🏻😀





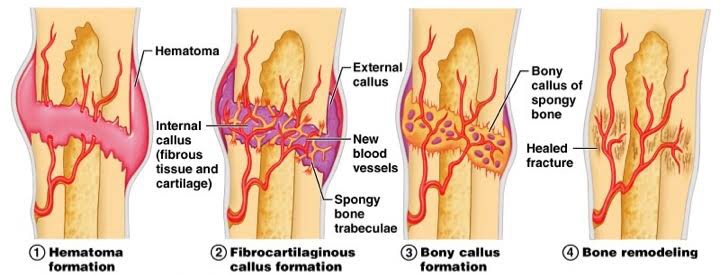
Dr. Mehnaz Memon🖊
Summary💡
🔅What are the 4 stages of bone healing?
•Hematoma formation
•Fibrocartilaginous callus formation
•Bony callus formation
•Bone remodeling
🔅What is callus formation in bone healing?
•Bone production begins when the clotted blood formed by inflammation is replaced with fibrous tissue and cartilage (known as soft callus). As healing progresses, the soft callus is replaced with hard bone (known as hard callus), which is visible on x-rays several weeks after the fracture.
🔅What foods heal bones faster?
•Iron helps your body make collagen to rebuild bone. It also plays a part in getting oxygen into your bones to help them heal.
•Good sources: Red meat, dark-meat chicken or turkey, oily fish, eggs, dried fruits, leafy green veggies, whole-grain breads, and fortified cereals.
🔅How long does it take for a broken bone to fully heal?
•A broken bone and the surrounding soft tissue damage need a minimum of six to eight weeks to heal. However, depending on your general health and the condition of your bone and soft tissue, healing can take much longer.
References:

🔍Tap to View in full size!




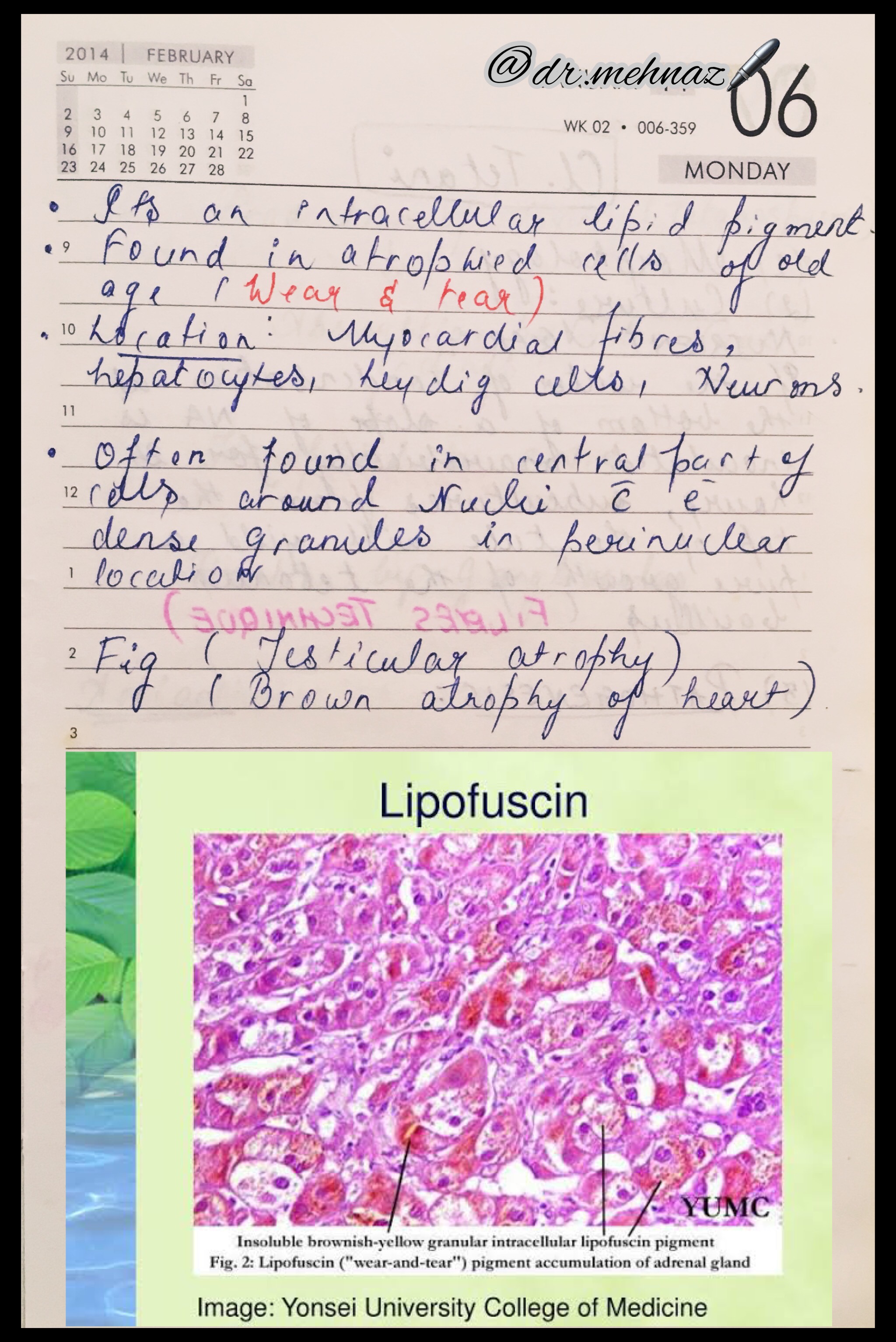

Dr. Mehnaz Memon🖊
References: Textbook of Pathology, Harsh Mohan; Random google Images

(i) Hypotensive States: (Shock, Spinal Anaesthesia)
➡️ In case of anaphylactic shock or angioedema of Larynx or for bronchospasm attending drug hypersensitivity (Adrenaline + sub-class of gluco-corticoids) is recommended.
(ii) Along with local anaesthetic:
➡️ Adrenaline 1 in 2,00,000 to 1 in 1,00,000 for infilteration, nerve block, spinal anaesthesia
🔅Effects:
(iii) Control of local bleeding: (Skin, mucous membrane eg. Epistaxis)
➡️ Compresses of adrenaline 1 in 10,000 can control arteriolar & capillary bleeding
🔅Cardiac Arrest (Drowning, Stokes-Adam syndrome)
👉🏻 Adrenaline is used to stimulate the heart, i.v infusion with external cardiac massage
👉🏻 The ester prodrug of adrenaline – Dipivefrine is an adjuvant drug for open angle glaucoma
👉🏻 Adrenaline can be used as an expedient measure but glucose should be given as soon as possible.
Dr. Mehnaz Memon🖊
References: Essentials of Medical pharmacology, KD Tripathi (7th Ed)

🔅The American Association of Endodontics defines resorption as, “a condition associated with either physiologic or a pathologic process resulting in a loss of dentin, cementum, and/or bone. Vital tissue is necessary for either external or internal resorption to occur.”
🔅By this definition, internal resorption is “a defect of the internal aspect of the root following necrosis of odontoblasts as a result of chronic inflammation and bacterial invasion of the pulp tissue.”
🔅External resorption is “resorption initiated in the periodontium and initially affecting the external surfaces of the tooth—may be further classified as surface, inflammatory, or replacement, or by location as cervical, lateral, or apical; may or may not invade the dental pulpal space.”




Dr. Mehnaz Memon🖊
References:
Tap to View 👇🏻


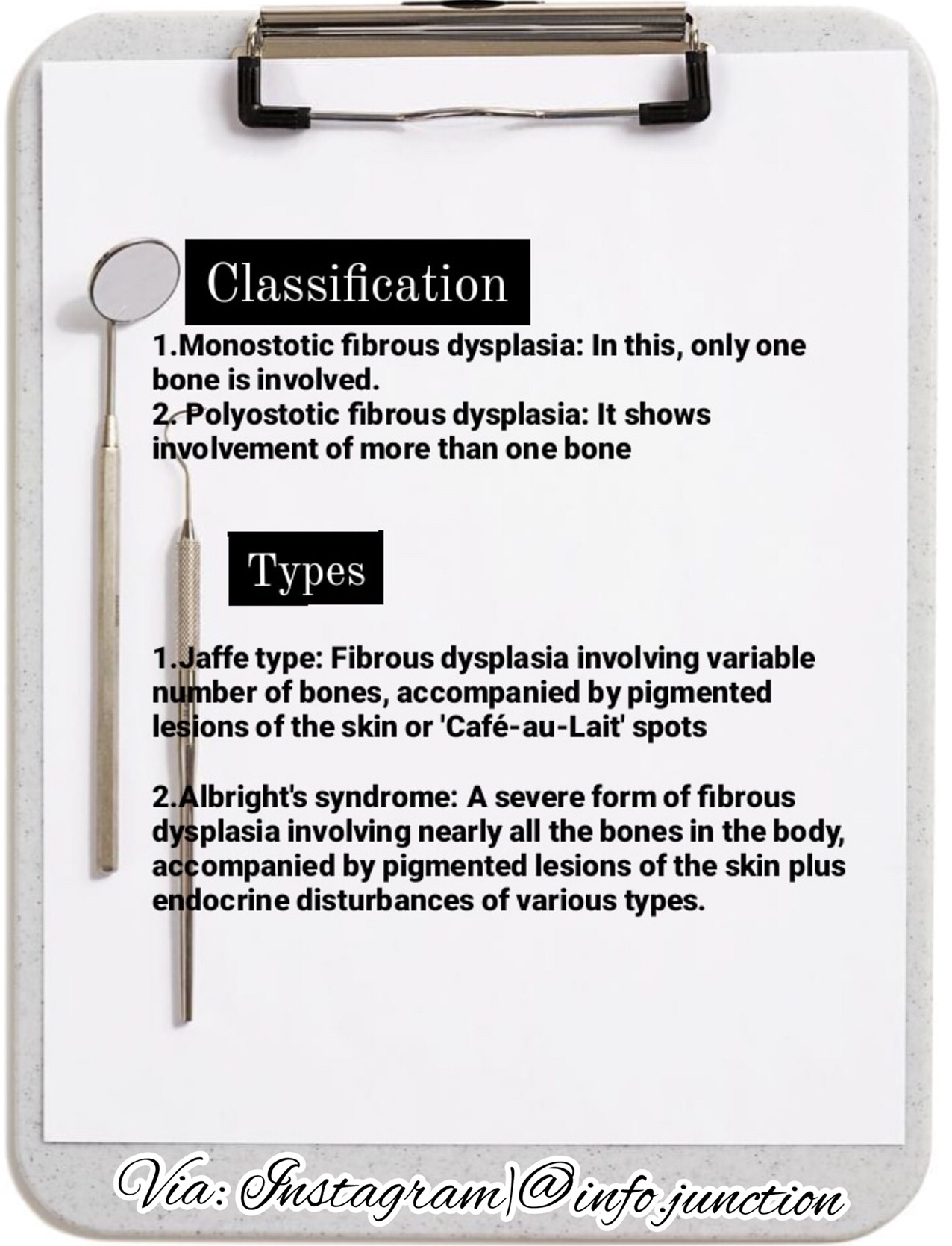



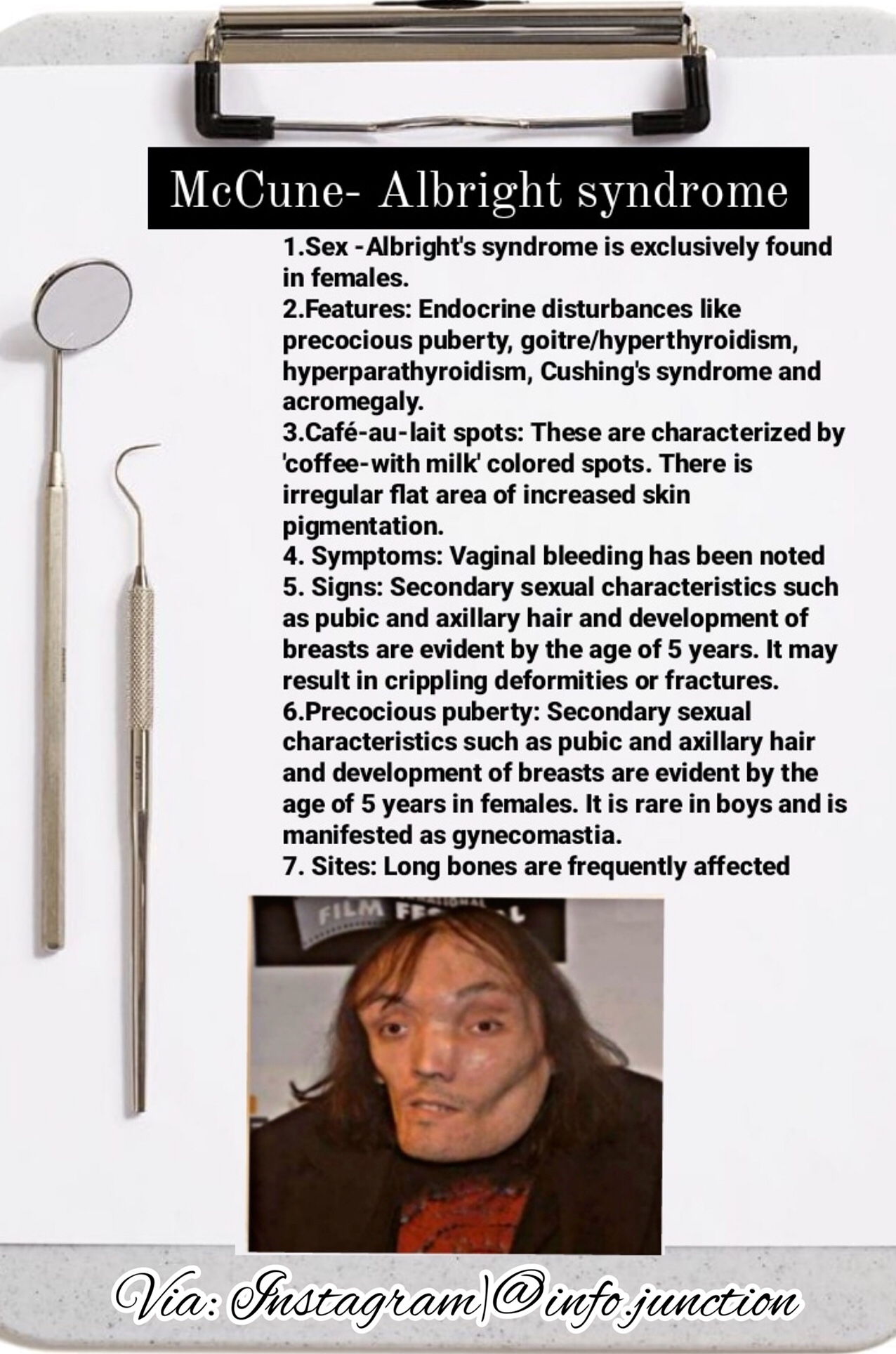




Dentowesome 2020📖📝
Canine retractors are springs that are used to move canine in a distal direction.
1. Based on location
2. Based on presence of helix or loop
3. Based on mode of action
▪️BUCCAL CANINE RETRACTOR:
INDICATION: Is used where a buccally placed canine has to be moved palatally as well as distally.
TYPES:
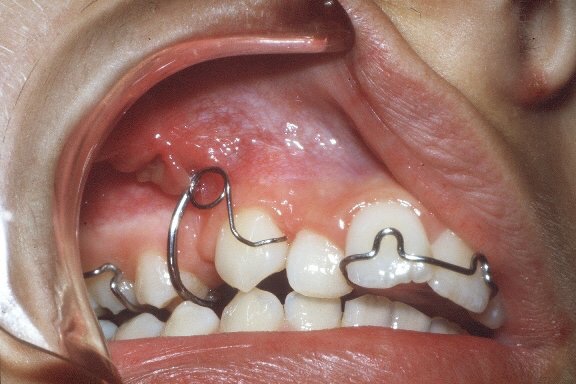
• Self supporting or unsupported
• Supported
▪️SELF SUPPORTED BUCCAL CANINE RETRACTOR:
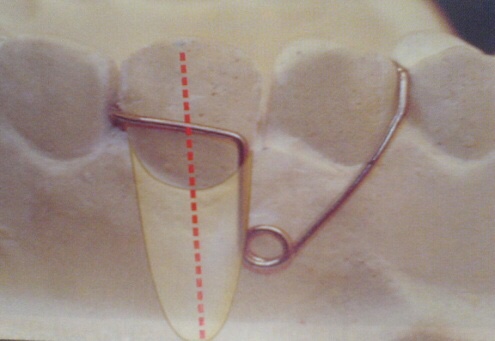
DESIGN & CONSTRUCTION
ACTIVATION
👉🏻The spring should be activated by only 1mm. Only spring which is activated by closing the coil
👉🏻Distal activation- It is effected at the coil by bending the anterior limb over the round beak of a pair of spring forming pliers
👉🏻Palatal activation- It is undertaken in the anterior limb after it emerges from the coil
DISADVANTAGES
▪️SUPPORTED BUCCAL CANINE RETRACTOR:

DESIGN
ACTIVATION
▪️AN APPLIANCE TO RETRACT BUCCAL CANINE
Indication
▪️SOLDERED AUXILIARY SPRINGS TO MOVE A CANINE PALATALLY
• It is possible to solder a spring{0.7mm wire} to the bridge of the adams clasp on a first molar.
• The spring can be used to tuck an outstanding canine
Advantages
Disadvantages
▪️REVERSE LOOP BUCCAL RETRACTOR:
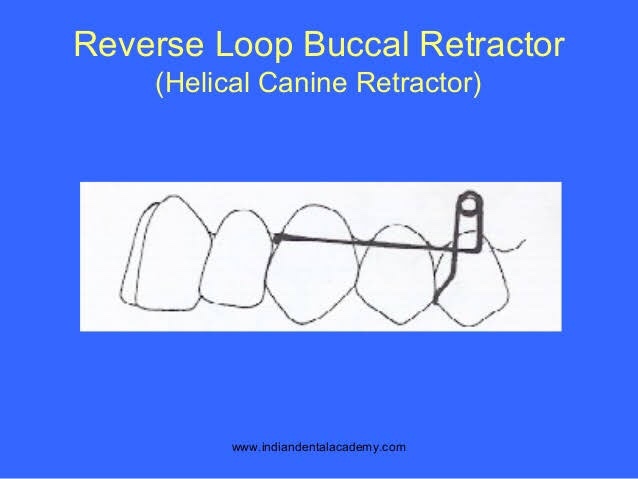
INDICATION
DESIGN
ACTIVATION
DRAWBACKS
• It is stiff in the horizontal plane yet very unstable vertically
▪️An appliance to retract lower canine
Indication
Anterior crowding
Active component
Reverse loop buccal retractor
Retention
Adams clasp on 6|6
Baseplate
A lingual bar rather than acrylic in the incisor region
Anchorage
Clasped teeth
Teeth and alveolar process contacted by the appliance
▪️U loop canine retractor
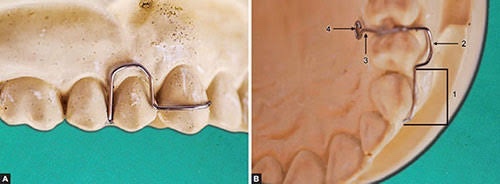
INDICATIONS
DESIGN
ACTIVATION – Close the loops by 1mm or free end is cut by 1mm & it is readapted on to the mesial side
DRAWBACKS – Requires frequent adjustments
▪️AN APPLIANCE TO MOVE A CANINE OCCLUSALLY
Indication – Partially erupted canine
Active component – U loop canine retractor, engages a hook bonded to the buccal surface of the canine
Retention – Adams clasp on 6|6
Baseplate – As much palatal coverage as the canine position permits to offer max. resistance to the occlusally directed force
Anchorage – Acrylic in the palate
▪️Buccal acrylic appliance to retract lower canine
Indication – To overcome the dual problems of limited space for tongue & poor retention provided by adams clasp
Active component – Buccal canine spring 0.7mm
Retention – Lingually placed jacksons clasp on the first molar [to overcome the problem of limited undercut on the buccal aspect of lower molars, appliances have been described with clasping on the lingual aspect of molars BELL 1983]
Baseplate – 2 segments of acrylic 1-2mm from the buccal mucosa. These are connected in the midline by a heavy ss bar, {2mm x 1mm}oval in cross section lying close to buccal mucosa below the lower incisors
Anchorage – First molar, with minimal anchorage effect from acrylic
▪️PALATAL CANINE RETRACTOR:

INDICATIONS – In cases where canine is placed palatally & requires distal & buccal movement
DESIGN
ACTIVATION – By opening the coil by 2-3mm where the active arm emerges out of the coil
▪️CONCLUSION:
• For canine retractors whether buccal or palatal to be successful, it is important for the canines to be mesially angulated prior to treatment
• If the canine is normal & distally angulated prior to treatment, a removable canine retractor will cause an unsightly distal angulation of the canine at the completion of retraction which in turn will take a long time to correct with fixed appliance
• For this reason, use of removable appliance for canine retraction is declining as fixed appliance have greater control over tooth movement
References:
A chronic, autoimmune, sub-epidermal blistering skin disease that rarely involves mucous membrane.

Age: Elderly (>60 years)
Skin Lesions:
Oral Manifestations:
Vesicles appear gingivally👇🏻
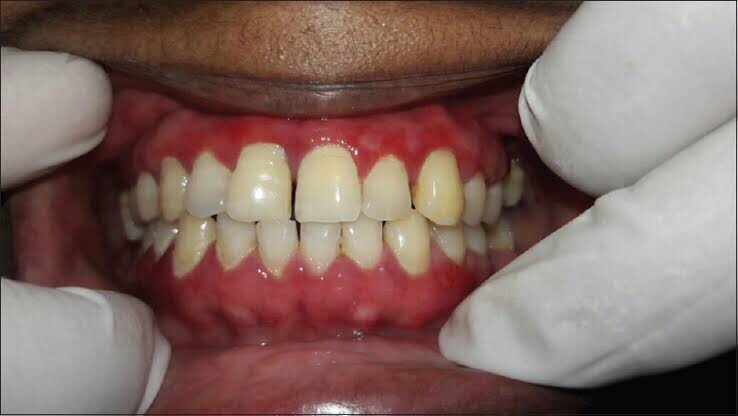
Erythematous & desquamate as result of minor frictional trauma
👉🏻 Oral lesions comprise of bullae/vesicle that rupture to form erosions and ultimately leave out ulcerations
👉🏻 Other sites:
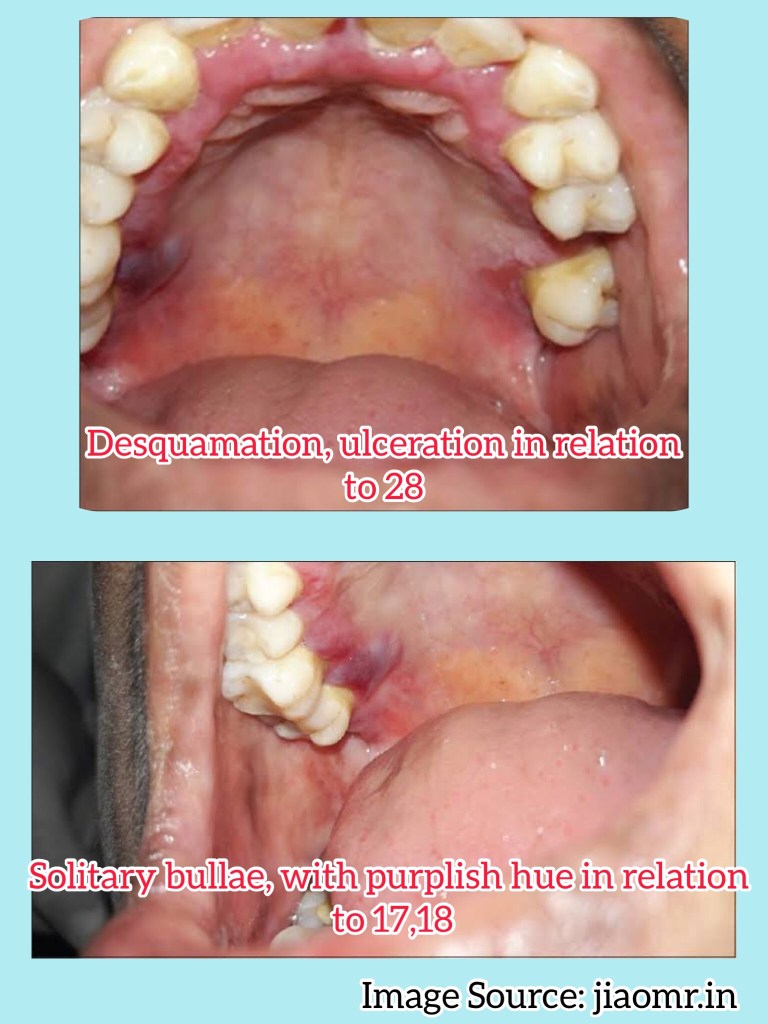
Apart from evaluating history, clinical presentation, histopathological analysis is carried out followed by direct immunofluorescence study for the differential diagnosis and confirmation of the condition.
👉🏻Histopathology:
👉🏻Direct immunofluorescence is found to be the gold standard test. Deposition pattern of different types of immunoreactants differentiates the various immune-mediated diseases. Direct immunofluorescence shows presence of IgG and C3 deposits along the basement membrane zone.
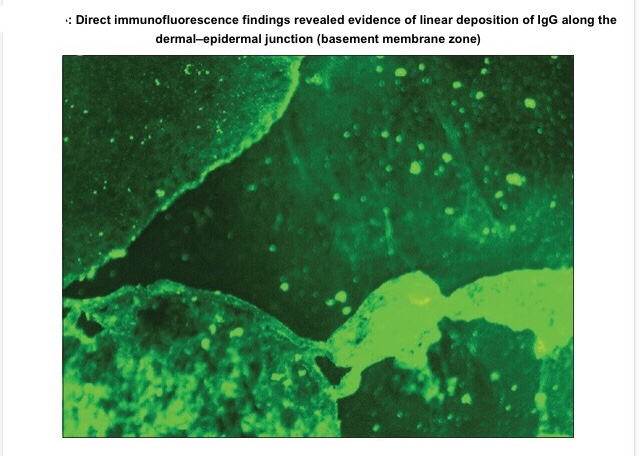
👉🏻Electron Microscopy: In bullous pemphigoid (BP), the 180 kD antigen (BPAG2) was shown by immuno-EM to be a transmembrane molecule and to possess an autoantibody binding site outside the cell, suggesting a major pathogenic role for the BPAG2 in blister formation.
• Mucous membrane pemphigoid can be differentiated from BP by its predominant involvement of mucosal surfaces and positive Nikolsky’s sign.
• Lichen planus pemphigoides is clinically differentiated by the presence of lichen planus lesions in addition to tense blisters.
• Nikolsky’s sign is present in case of pemphigus and cicatricial pemphigoid, but not in the case of BP.
👉🏻Treatment is based on the degree of cutaneous and oral involvement. Mostly, topical steroid (clobetasol propionate) gives satisfactory result in case of smaller area of skin involvement, whereas larger area of skin involvement and recurrent cases are treated satisfactorily with systemic steroids and immunosuppressive agents.
👉🏻Recommended dosage for oral prednisolone is 0.3–1.25 mg/kg body weight/day, controls disease within 1–2 weeks, followed by which the dose is tapered. Dexamethasone (100 mg in 500 mL 5% dextrose i.v. over 2–3 h for three consecutive days) is the preferred steroid for pulse therapy, either administered alone or in combination with cyclophosphamide.
Other drugs for treating BP include new antibody modulators, rituximab 375mg/m2weekly over 4 weeks and omalizumab subcutaneously 300–375 mg for every 6 weeks.
👉🏻Higher doses of systemic corticosteroids seem to be associated with higher mortality rates, which led to the addition of corticosteroid-sparing agents to the treatment of BP. The most frequently used immunosuppressive agent is azathioprine (0.5–2.5 mg/kg body weight/day). Others being cyclophosphamide, methotrexate, cyclosporine A, combination tetracycline/minocycline along with nicotinamide, and more recently, mycophenolate mofetil, a DNA synthesis inhibitor, and methotrexate, a folate antagonist.
👉🏻IVIg – A dose of 1–2 g/kg for five consecutive day cycle of 0.4 g/kg/day, although a 3-day cycle may be used in cases that are nonresponsive to conventional therapy.
Dr. Mehnaz Memon🖊
References: