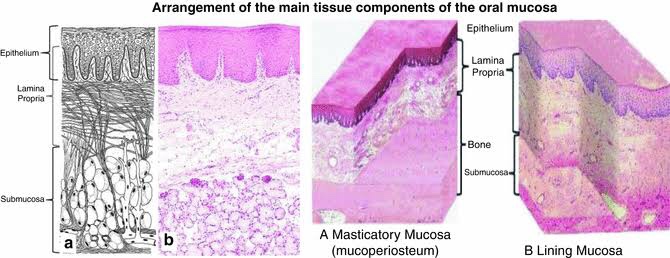
🔹Enamel:
➡️ The periapical expressions of pathologic Amelogenesis are hypoplasia, which is manifested by pitting, furrowing or even total absence of enamel & hypocalcification in the form of opaque or chalky areas on normally contoured enamel surfaces.
➡️ It is caused by systemic, local or hereditary factors
➡️ An example of systemic type of calcification of the enamel is so called Mottled Enamel
➡️ High flouride content in water – deficiency to calcify
➡️ The discoloration of the teeth from administration of tetracyclins during childhood is very common clinical problem
🔹 Dentin:
➡️ Dentin sensitivity of pain is exlained by hydrodynamic theory, the alteration of the fluid & cellular contents ending in contact with these cells.
➡️ Erosion of peritubular dentin & smear plug removal accounts for dentin hypersensitivity caused by agents like acidic soft drinks.
➡️ The rapid penetration & spread of caries in the dentin is the result of the tubule system in the dentin
➡️ Electron microscope of carious dentin show regions of massive bacterial invasion of dentinal tubules.
➡️ Smear layer consist of cut dentin surface which occludes the tubules & reduces permeability. Also prevents adhesion of restorative materials to dentin. Therefore this layer is removed by etching.
🔹 Cementum:
➡️ Cementum is more resistant to resorption than bone. It is for this reason orthodontic tooth movement is made possible.
➡️ Cementum resorption can occur after trauma or excessive occlusal forces. After resorption has ceased the damage usually is repaired either by formation of acellular/cellular cementum or alternate formation of both.
➡️ In most cases of repair there is tendency to re-establish the former outline of the root surface. This is called anatomic repair.
➡️ It is only a thin layer of cementum is deposited on the surface of resorption, the root outline is not reconstructed & a baylike recess remains. This is termed functional repair.
➡️ Hypercementosis – secondary to periapical infammation or extensive occlusal stress. Extraction of such tooth may necessitate the removal of bone.
Source: Internet
Dentowesome 2020 @dr.mehnaz