A 26-year-old patient presented with a rapidly growing lesion that expanded the maxilla. There was bone destruction on the radiograph and therefore malignancy was suspected. On biopsy, the lesion was intraosseous and was cavitated. There was profuse bleeding and a small biopsy of the lining was taken. The pathologist reported osteoclast-like giant cells and granulation tissue with blood clots.
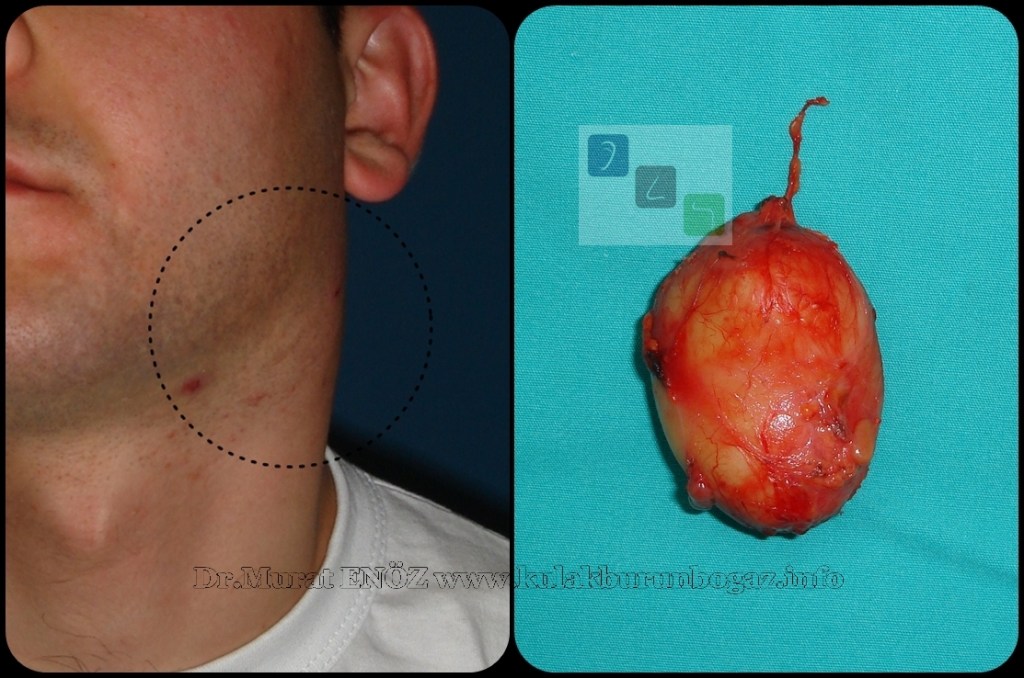
Branchial or lymphoepithelial cysts are typically present in the second and third decades after slow enlargement. They are lined by squamous epithelium and have lymphoid tissue with prominent follicles in the wall. In older patients, they may be confused with cystic metastatic squamous carcinoma in a lymph node. Metastatic thyroid cancer can also mimic branchial cysts. The cyst must be carefully examined by the pathologist.
RESEARCH PAPERS
- Branchial or lymphoepithelial cysts are a type of congenital neck pathology that can occur due to the remnants of a branchial arch developing into a cyst, causing swelling [9].
- These cysts are also known as branchial cleft cysts [1][3][6][7][9][10].
- The prevalence of branchial cysts in children is reported to be around 24.2% [2].
- They can occur in various locations, including the submandibular gland, parotid gland, and palatine tonsil [1][4][8][10].
- The etiopathogenesis of these cysts is still a subject of debate, and various postulations have been made regarding the matter [8].
- Thyroid lymphoepithelial cysts are reported to originate from follicular cells and are unrelated to solid cell nests and lateral cervical cysts arising from branchial-derived remnants [5].
- There is no specific reference available that discusses branchial cysts in the maxilla. However, branchial cysts are typically found in the lateral neck region, deep to the sternocleidomastoid muscle, and are derived from remnants of the branchial apparatus [13][15][16].
- They are congenital anomalies that usually present as a cystic mass in the neck [17].
- In rare cases, branchial cysts can arise in the posterior mediastinum [11].
- The classification of branchial cysts depends on the branchial cleft they originated from, with locations ranging from the external auditory canal to the lower part of the neck [12].
- Branchial cysts are typically diagnosed based on clinical examination and imaging studies, such as ultrasound or computed tomography [13].
- Treatment usually involves surgical excision of the cyst [14].
REFERENCES
- [1] Ahamed, Kannan, Velaven, Sathyanarayanan, Roshni, E (2014). Lymphoepithelial cyst of the submandibular gland. J Pharm Bioall Sci, 5(6), 185. https://doi.org/10.4103/0975-7406.137464
- [2] Irani, Zerehpoush, Sabeti (2016). Prevalence of Pathological Entities in Neck Masses: A Study of 1208 Consecutive Cases. Avicenna J Dent Res, 1(8), 4-4. https://doi.org/10.17795/ajdr-25614
- [3] Delantoni, Onder, Orhan (2022). B-mode and color Doppler imaging of different types of branchial cleft cysts in children. A multicenter study and review of the literature. J Ultrason, 90(22), 174-178. https://doi.org/10.15557/jou.2022.0028
- [4] Som, Brandwein, Silvers (1995). Nodal inclusion cysts of the parotid gland and parapharyngeal space: A discussion of lymphoepithelial, aids-related parotid, and branchial cysts, cystic warthin’s tumors, and cysts in sjogren’s syndrome. Laryngoscope, 10(105), 1122-1128. https://doi.org/10.1288/00005537-199510000-00020
- [5] Suzuki, Hirokawa, Ito, Takada, Higuchi, Hayashi, … & Miyauchi (2018). Derivation of thyroid lymphoepithelial cysts from follicular cells. Endocr J, 5(65), 579-586. https://doi.org/10.1507/endocrj.ej17-0402
- [6] Najib, Berrada, Lahjaouj, Oukessou, Rouadi, Abada, … & Mahtar (2021). Cervical lymphoepithelial cyst: Case report and literature review. Annals of Medicine and Surgery, (61), 185-187. https://doi.org/10.1016/j.amsu.2020.12.041
- [7] Gill, Chhabra, Singh, Mehrotra, Rawat (2020). Lymphoepithelial Cyst, A Diagnostic Dilemma: Case Report. Ann of Pathol and Lab Med, 10(7), C137-140. https://doi.org/10.21276/apalm.2824
- [8] Gurka (2020). Case Report of a Parotid Benign Lymphoepithelial Cyst. ADOH, 3(12). https://doi.org/10.19080/adoh.2020.12.555836
- [9] Park, Yoon, Bang, Ahn (2019). Branchial cleft cyst in the parotid gland in a human immunodeficiency virus-negative patient. Arch Craniofac Surg, 3(20), 191-194. https://doi.org/10.7181/acfs.2019.00031
- [10] Bingöl, Balta, Bingöl, Mazlumoglu, Kilic (2016). Lymphoepithelial Cyst in the Palatine Tonsil. Case Reports in Otolaryngology, (2016), 1-3. https://doi.org/10.1155/2016/6296840
- [11] Han, Shang (2023). Branchial cleft cyst arising in posterior mediastinum: A case report. Front. Surg., (9). https://doi.org/10.3389/fsurg.2022.1088142
- [12] Park, Yoon, Bang, Ahn (2019). Branchial cleft cyst in the parotid gland in a human immunodeficiency virus-negative patient. Arch Craniofac Surg, 3(20), 191-194. https://doi.org/10.7181/acfs.2019.00031
- [13] Reynolds, Yap, Marikar, Roland (2019). Fifteen-minute consultation: The infant with a neck lump. Arch Dis Child Educ Pract Ed, 5(105), 258-261. https://doi.org/10.1136/archdischild-2019-316827
- [14] Dhoke, Khadakkar, Dhote, Choudhary, Harkare, Kamal (2012). Type III Second Branchial Cleft Cyst. International Journal of Head and Neck Surgery, 2(3), 112-114. https://doi.org/10.5005/jp-journals-10001-1107
